Category: Uncategorized
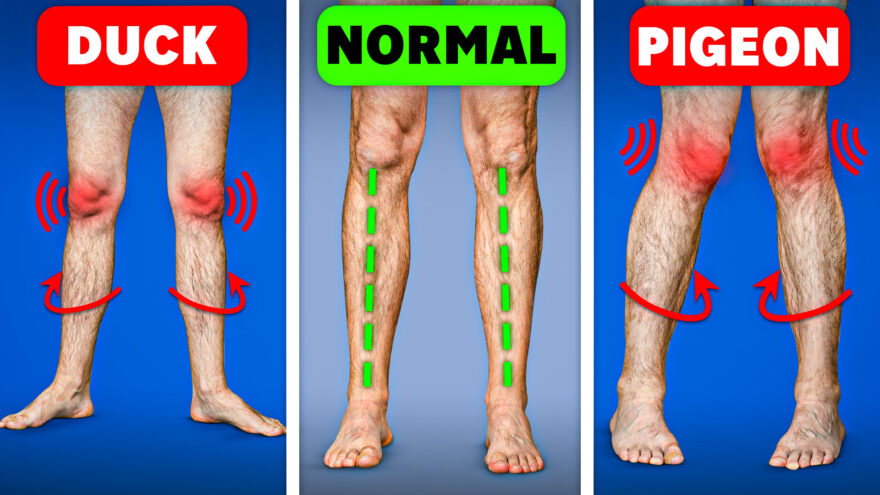
Fix Duck and Pigeon Feet FAST
A Comprehensive Foot Posture Guide Do you ever notice someone walking with their feet turned out like a duck or…

5 Exercises That Fix 90% of Problems
Unlock Your Mobility: 4 Common Movement Issues and Exercises to Fix Them Mobility issues, pain, and tension often boil down…

The Last Diaphragmatic Breathing Post You’ll Ever Need
Master diaphragmatic breathing for better health, mobility, and performance. Understand the mechanics of breathing, how different breathing styles impact your…

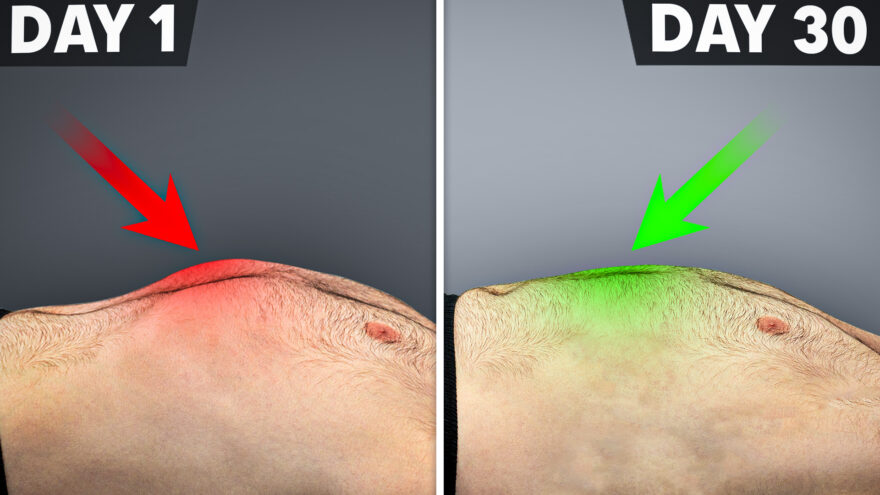
5 Exercises That Heal the Body
Discover how to alleviate pain and improve mobility with these five tension-reducing exercises. Perfect for enhancing movement fluidity and reducing…
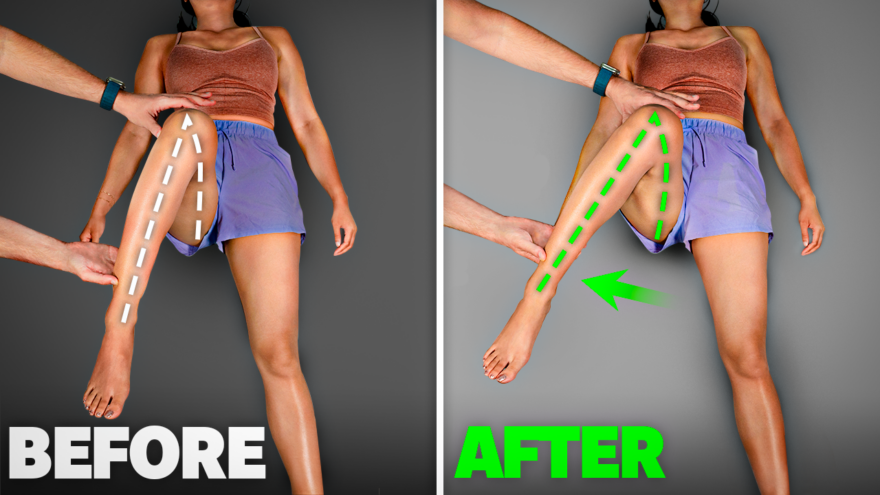
Fix 90% of Hip Problems in 30 Days
Discover effective exercises to fix all your hip problems in just 30 days! Learn how to test your hip mobility…
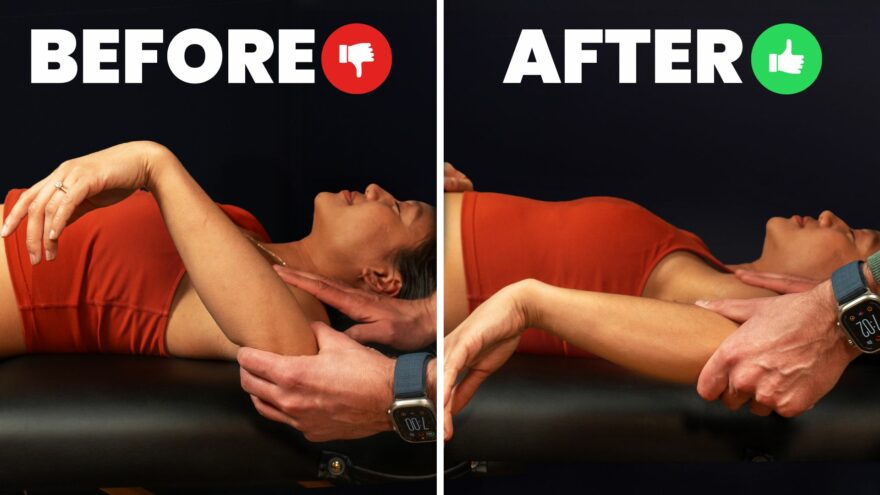
Fix Your Shoulder Internal Rotation FAST
Meta Description: Unleash your shoulder’s full potential! Discover simple yet effective exercises to rapidly improve shoulder internal rotation, enhancing your…

Unlock A Deeper Squat (You Haven’t Tried This)
Learn how to squat deeper with our comprehensive guide. Understand the biomechanics, importance of sacral counter-nutation, and exercises to improve…
The REAL Reason Tim Ferriss Has Lower Back Pain
im Ferriss’ battle with back pain decoded! Dive deep into the overlooked connection between hip dynamics and lower back discomfort.…

Why Jordan Peterson Saying Standing Up Straight is WRONG
Debunking the myth of “Stand Up Straight with Your Shoulders Back” by Jordan Peterson. Learn why this posture can be…

DON’T Start Plyometrics Unless You Do THIS
Most people start with the wrong jumps Are you ready to jumpstart your strength and force production? Look no further…
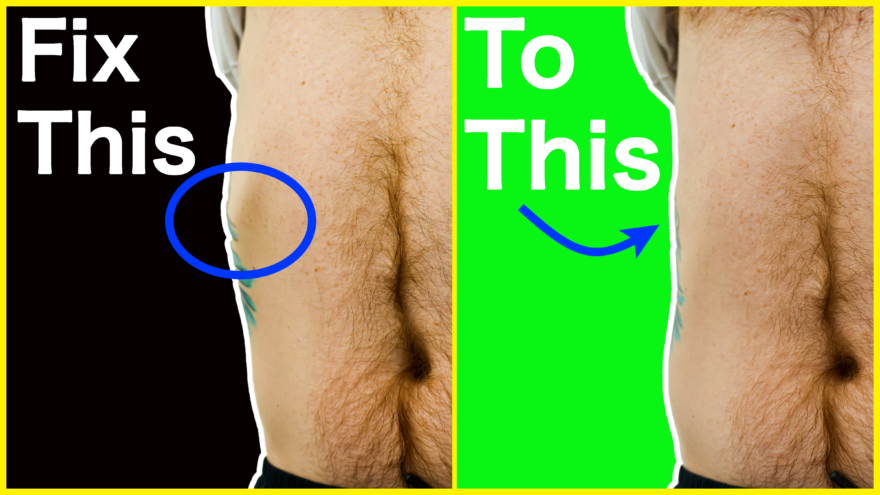
Uneven Rib Flare – Fix it For Good
Why does my ribcage protrude on one side? If your rib cage appears extra pointy on one side compared to…

What REALLY is Good Posture?
Is there such a thing? There’s a common misconception within the movement space that good posture is this one position…

Oblique Sit Press – EVERYTHING You Need to Know!
The best overhead press starting point? Overhead pressing is SUPER tough to learn. In fact, most people won’t have adequate…

Top 10 Posts of 2021
The posts the fam loved the most! At the end of each year, I like to see what you wonderful…