Table of Contents
If you mouth breathe, struggle sleeping, snore, or have eustachian tube issues, then check this out!
Mouth breathing is linked to sleep disorders, tooth decay, eustachian tube issues, and so much more, what do you do about it?
Could the answer be myofunctional therapy? That’s what I sift through with Myofunctional therapist Melissa Mugno.
In this podcast, you’ll learn:
- Why Steph Curry chews on his mouthguard the way he does
- Why do we clench and grind our teeth?
- The importance of breastfeeding on orofacial development
- What myofunctional therapy is and where it belongs in the healthcare system
- The two causes of the mouth breathing epidemic and how to tackle this problem
- How behavior change plays a crucial role in a successful outcome
- The intersection of physical and myofunctional therapy
- Why belly breathing is totally overrated
- The myofunctional therapy intervention process
- The link between swallowing and eustachian tube dysfunction
- and TONS more
If you are ready to make your upper airway healthy as can be, then definitely check this podcast out.
Look below to watch the interview, listen to the podcast, get the show notes, and read the modified transcripts.
and the audio version:
Learn more about Melissa
Since becoming an Orofacial Myofunctional Therapist in 2014, Melissa has improved the lives of hundreds of patients and lectured around the country. Melissa treats patients of all ages suffering from a wide range of conditions stemming from adverse myofunctional habits. Her background as a Dental Hygienist and experience in the fields of Orthodontics and Pedodontics contributes to her success. Melissa works in Las Vegas, NV, and is a Breathe Associate at The Breathe Institute in Los Angles, CA.
Show notes
Here are links to things mentioned in the interview:
Joy Moeller – One of the foundational people in the field of myofunctional therapy.
Sandra Coulson – Another foundational person in myofunctional therapy.
Myobrace – A possible way to improve teeth position.
Dr. Tara Erson – A great dentist in Las Vegas![]()
Dr. Hockel – My dentist who is doing my palatal expansion.
Dr. Kareen Landerville – She is my go-to optometrist in Las Vegas
The Breathe Institute – Where I got my tongue-tie release done.
Dr. Soroush Zaghi – The doctor who did my tongue-tie release.
AOMT – That’s who I took my myofunctional therapy course through. You can peep the review here.
Bill Hartman – Daddy-O Pops himself. My mentor.
The Enduring Impact of What Clinicians Say to People With Low Back Pain – A great article that goes into how maladaptive beliefs can manifest.
Modified Transcripts
Why Steph Curry chews on his mouthguard
Zac Cupples: So, Steph Curry walks into your office, and he asks you, hey, Melissa, why is it that I like to chew on my mouth guard so much?
Melissa Mugno: So, the chewing is because of his airway.
Zac: Mm-hmm. Do tell. Tell me more.
Melissa: So, in sleep dentistry or airway, we’ve really come full circle to understand that like chewing and clenching, has a lot more to do with a deficiency in the airway than it does anything else.
So, there are habits that are created, that actually kind of stimulate the jaw to come forward, and there’s a feeling that feels good. It gives us more air, more serotonin overall, and it actually will give you a lot more clarity.
Get some good oxygen, you feel better. So that’s actually what’s happening. So, the chewing couple times you do it, you’re like, it feels good, right? Most humans continue to do things that feel good, stop doing things that feel bad. So, please stop doing that.
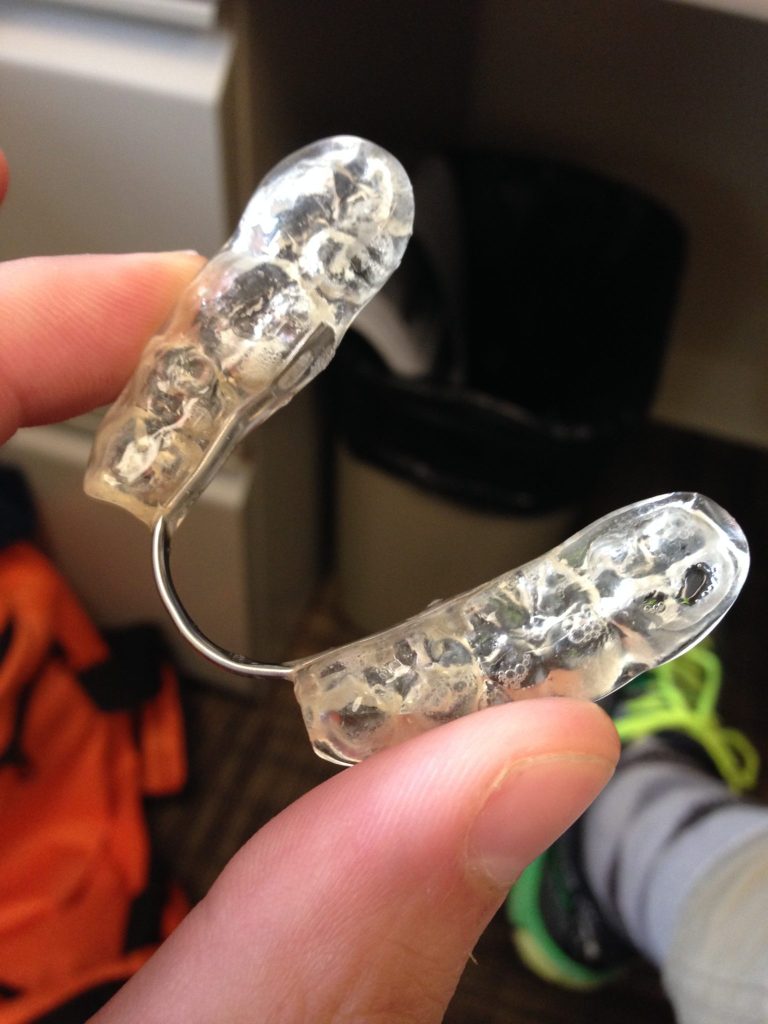
But the thing was, Steph Curry that’s quite interesting is he doesn’t just chew on it. He doesn’t even – more interesting, he flips it out of his mouth and holds it. And what I was saying to you before was, again, I have not worked on Steph Curry so I do not know. This is just me looking at it, I was intrigued by it.
My husband brought it up and said, ‘’Hey, this guy’s really known for doing this’’ and I was interested. I’ve always thought there was a big sports connection. I started looking at how thick his mouth guard was and I’m like, “oh, it’s at least two millimeters, two and a half.”
One of the things we do, the dentist will do or to help patients that have sleep issues, is they’ll actually open up their bite, open up the jaw, so they can’t close all the way, which naturally will allow their jaw to come forward, and that does is it opens up the airway and allows for the air to flow easier. So, he’s holding it, and he’s protruding his own bite and you can see it’s literally bringing his jaw forward.
I started looking and then I watched some YouTube videos and I saw that Forbes I think it was? It might be off one of the bigger publications that did an actual survey or did some type of research of how many free throws that he made when the mouthguard was out versus when it wasn’t. He shot significantly better with it in!
It was a no-brainer to me. he’s breathing better.
Oxygen will absolutely get you focused and therefore he is more comfortable. So why wouldn’t you keep doing it? Yeah, so now it’s become this whole thing. Now, I guess like, tons of athletes do it and I was like, yeah, of course, yes, it protects your teeth, but there’s a lot more to it.
Zac: But when you’re clenching as well, how does that open up the airway then? Because I would think…
Melissa: Clenching and grinding are not opening up the airway. It’s a side effect of having a reduced airway.
I love my analogies. So, I call it the body’s fire alarm. And so, it triggers something and what’s happening is the body knows it’s getting a reduced amount of air, so it acts to check that. It’s going to create some type of function, some type of habit to make sure everything’s good down there. So, this, the grinding, and I have this little theory that we grind when we’re kids because we’re carefree and we clench when we’re older because we’re trying to control it.
Zac: Gotcha.
Melissa: It seems that way more adults clench than kids and I realized some of my, I mean, it’s not absolutely proven, but my adults that grind are usually my cool cats. They just grind it out, let that jaw flow. The adults are like they’re trying to control, they don’t want that feeling. It’s they’re trying to control that bite. They don’t know why their jaw wants to move. So, I believe the clenching has a lot to do with trying to control
Zac: Prevent it.
Melissa: Exactly. It’s also connected to the mind–anxiety and all like so much more mental health and stuff like that. I think it’s a natural thing that happens as we become adults that we just want to control.
Zac: Yeah.
Melissa: That control leads to me building some type of subconscious behavior, to take it out on, and activating the buccinators and we’re straining out all in here. No nasal breathing.
Breastfeeding
Melissa: That’s one reason why breastfeeding is so important.
Yes, it has a lot of cool nutrition value, but one of the coolest things is that happens is it actually teaches you how to breathe and eat at the same time.
The tongues pushes the nipple up, and then be able to help extract the milk, and then the baby’s actually letting the mom’s body know, hey, you got to keep producing.
When moms don’t produce milk, they automatically assume it’s their fault because they have mom guilt. So, then it’s like, I just got to make my baby free to be able to eat and stuff. And they think that the formula is doing the trick but what’s not happening is that then the bottle goes in, and now the tongue goes down.
Zac: Then you can’t control the rate at which the liquid is coming in when it’s a bottle versus when you’re breastfeeding.
Melissa: Then nipple companies make it go quicker, the older you get, make it easier, it just flow it in there, no work needed.
Then we don’t learn how to breathe nasally really young, then problems ensue.
Teeth clenching and grinding
Zac: From my standpoint, when we see someone clenching or grinding on the PT side of things, usually that’s done to restrict available movement. So, you almost make the system more rigid. And to your point when you’re talking about who is this it’s those type-A people and a lot of times, I forget what book it was where they talked about the chairs in the waiting room of a cardiologist.
Melissa: Oh, yes in the armrests. Yeah, because like they’re gripping way hard; fight or flight.
Zac: Yeah, and maybe it’s just to change the pressurization that’s going on in the airway.
The importance of breathing
Melissa: I laugh a little bit when people will be like, airway dentistry, PT, speech, what has that have to do with it? “I’m like, Oh, yeah. Who needs air?” Oh, we don’t have enough research and I just want to be silly and be like, so we don’t have enough research on how important oxygen is? Or seeing the interconnectivity of the body? We all heard that elbow bone is connected to the wrist bone song as a kid, right?
Zac: Yeah.
Melissa: I just paid you to tell me to breathe? I am breathing! Well, I mean, that’s left to be decided, right?
Myofunctional therapy
Zac: Well, and I think most people don’t even know that your specialty exists; myofunctional therapy.
Melissa: I don’t know if I’m the best representation of myofunctional therapists.
Zac: You’re just my favorite.
Melissa: Because it’s been more about connecting the dots for me and I think myofunctional therapy happened to be a vehicle that I could I drive that allowed me to go to all these places and I don’t think that would maybe be the same for most. I think most love the skill and the passion of myofunctional therapy and what it is a day in and day on and how to make the exercises better and that one on one with the patient.
I love my patients, don’t get me wrong but it’s more of this bigger thing for me. I like looking at the teeth, tongue, and more. It opens the door to another place. It’s probably my ADHD.
The beginning of my journey was untraditional. I was an orthodontic assistant for a long time, hygiene, whatever but I ended up not really even practicing all. My real calling was running a business, selling dental stuff, and making sure the patient and being that liaison to connect everything but at the end of the day, what does that mean? It means making sure the numbers and production and collection were good and I was good at that.
We had this really amazing pediatric dental program, but we had this hole in our practice. We would get these referrals for kids who we couldn’t start because they didn’t have all their molars in yet.
How do I make that work?
So long story short, I’m from New Jersey, we don’t have a very long summer there. And the doctor comes in and he’s like hand me this thing and he’s like, we’re going to go to this course, I’m like, in August in New Jersey, no, thank you, and ended up being a Myobrace course.
There was this patient with a Class III bite (where maxilla is behind the mandible). These presentations can occur either genetically or because the tongue sits low, pushing the jaw forward instead of the maxilla. The only real way to fix it is to do surgery (or so I thought).
Zac: Yeah, a lot of times they’ll break the jaw and pull it back.
Melissa: Yes. That’s a whole other thing.
Zac: I had a friend who did that and I didn’t know him at the time. He was a coworker and I told him ahead of time, my buddy was like, don’t do this. If anything, you got to bring the jaw forward.
Melissa: Did you know that? This was before you started doing?
Zac: Yeah.
Melissa: so, you were already?
Zac: Yeah. I knew like a little bit of airway stuff and like some of my earlier things, it was more about using splints to change occlusion. I started with a gelb splint.
Melissa: Really?
Zac: Yeah, because my wisdom teeth were still in and I had no truce of movements in the jaw and so we use the Gelb to try to get me a little bit extra just for moving perspective but then the fix was to get the wisdom teeth taken out. So, then we went that route. I wasn’t really having sleep issues, then but as I got older, it was –
Melissa: Well, you did your sleep study show sleep apnea?
Zac: No, I got upper airway resistance syndrome.
Melissa: I wonder because of your athleticism and all those things that because you – elongation in the sense you did, it would look like you might be more of a sleep apnea patient, but really, you’re UARS? Apparently, you and I are in the same club.
Zac: I know right?
Melissa: So we had this mom who all three of her boys had an underbite. She challenged us and asked if there was really nothing I can do besides surgery?
We ended up implementing myobrace and started to notice some decent changes, but the execution was rough; we didn’t know what to look for and how to progress.
So, the journey then, long story short, kind of went in that I really started to crave the need of like, okay, who created these exercises? Where did they come from and that actually kind of brought me full circle to Sandra Colson and realizing she was a huge part of working with them. Her husband was an orthodontist, she was a speech therapist, and they were getting amazing results. Learning from her made sense to the cases we had that relapsed.
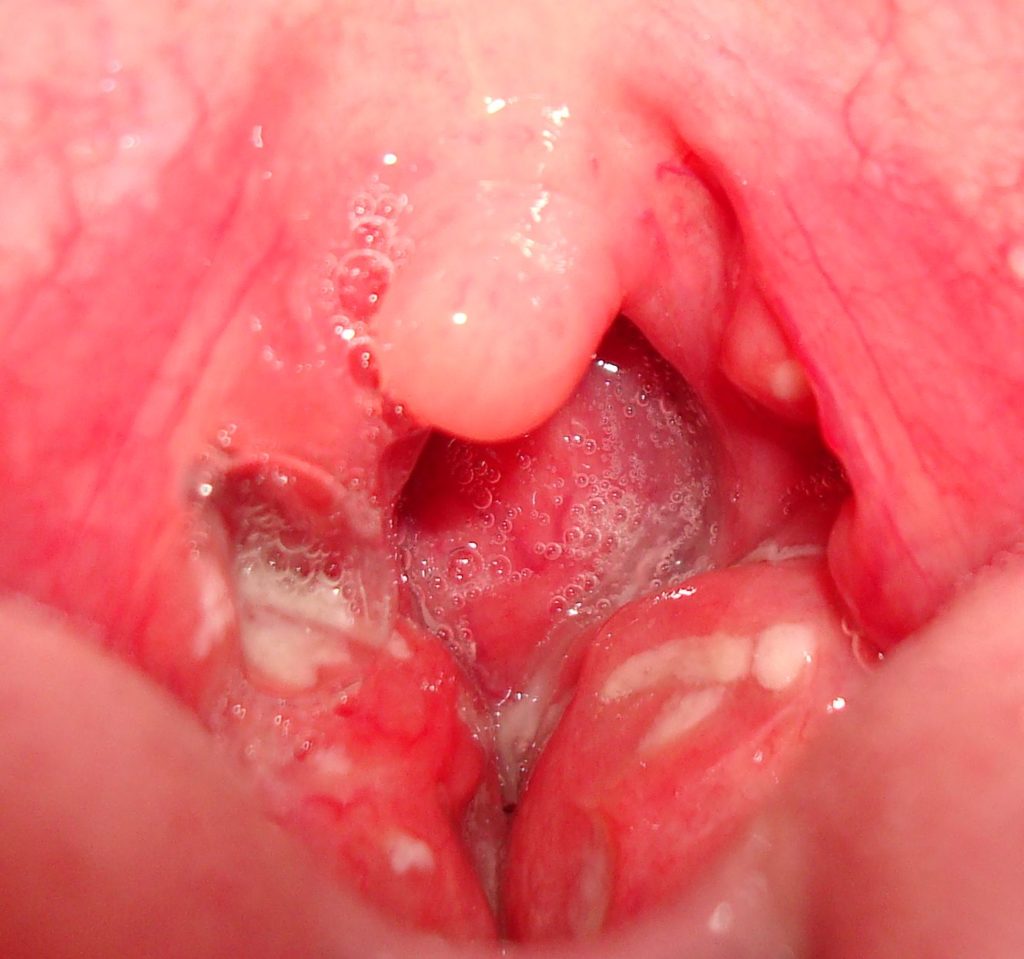
And it was important. I didn’t hear tonsils and adenoids so much like we weren’t bringing like was sort of doctors doing an orthodontist is doing his you know console, he’s usually rattling off stuff, that type of by you know, class one class two, upper post for your class or whatever, convex all the different profiles have any they might say, you know, within normal limits, but I noticed we started seeing WAY more enlarged tonsils.
My real aha moment was working with this amazing orthodontist who produced incredible smiles. It was my first job assisting, so I didn’t know any different, but he used removable appliances, nothing cemented.
Zac: Really?
Melissa: And we always were doing early expansion, twin blocks maras, we would use anything, everything was removable, prop that bite up, pull it forward, and expand the heck out of it.
Zac: Wow.
Melissa: Now he – how do I say this a nice way? He had, I guess back then I probably would have called an arrogance. He commanded the room. Right? Like you didn’t question. He just carried himself in a way. There was no option but the one he gave. Like if Bobby didn’t wear it. Like that’s your problem, then you shouldn’t make him wear like, so that level of expectation. So why that’s important to understand.
So, I go through and I remember one day we’re in the office and I know nothing, right? Like, I’m just figuring out how to do this. He walks by, and the patients are humble, we do and he’s like God, somebody should cut that kid’s tongue out of his mouth. It’s messing up my teeth.
It sounds dramatic but now I totally understand but I didn’t. I was like, wow, what a jerk. Right? Like, he doesn’t care. So, come all the way full circle, I’m now inMyobrace class, I’m doing it, and it was like this light went off, I was like, oh my gosh, this is what he was talking about. The kid was tongue-thrusting. No matter what he did to that bite, he couldn’t close it.
Zac: Because the tongue kept pushing on the teeth.
Melissa: Yes, that’s what he meant. He’s like God, that tongue is going to destroy everything. So, he knew it. But the crazy thing is if you go back into his story, he was originally an engineer. He was a mechanical engineer prior. Then after had gotten married, went back in dentistry and became an orthodontist.
Essentially, orthodontics is engineering. It’s all about force and movement and I think that’s what makes most orthodontists very specialized is because they can see things in a different way.
With Myobrace, we could take it to another level.
Years go by and I go back to school and all those things. And I noticed, almost every orthodontist just cements everything in and they just, I didn’t even know you cemented it. It allowed me to basically see all aspects of dentistry, and I needed this whole journey to see it. That myofunctional was the most powerful thing. Oh, that’s why the teeth keep relapsing because we didn’t address the tongue thrust or we didn’t retrain the tongue, we would maybe tell the kid hey, Bobby, try to put your tongue up or we put a habit in there or something.
Well, anyone that’s ever had a real habit, thought was very easy to overcome, right? Especially if you don’t even know why you’re doing it. And mouth breathing and tongue posture, I mean, if you’re drinking all the time, you kind of know what you’re doing is wrong, right? Well, you know what the culprit might be like this is what’s causing this? But if you don’t even know that it’s wrong to mouth breathe and have a low tongue posture, now I tell you, oh, you have a breathing issue. It’s because of your tongue. What? Like how do you do that? How do you fix that?
Zac: Especially considering how common mouth breathing is.
Melissa: Well look at how it’s changed. So, you look in Disney movies, so if you go back to like Snow White, the older ones, all of the characters are lips closed.
Zac: Really?
Melissa: And now you go to Frozen, she’s drooling with her mouth open.
Zac: Wow. I never even noticed that but that totally make sense. Like sleeping beauty, was she snoring?
Melissa: No, no, lips closed, breathing through.
Zac: If you have this epidemic of mouth breathing, and maybe this is where you are realizing the limitations of myofunctional therapy. Just like I have limitations as a PT that’s why I talk to you and work with a ton of other people who have skills that I don’t.
Where myofunctional therapy starts
Melissa: In a perfect world, you’d start with breastfeeding. Every baby that’s born would address whether or not the baby has a tongue-tie, and has a tongue tie to the new protocols and standards. Unfortunately, the system makes that hard. So now we go out longer and longer. Now, time starts dwindling. So that’s in the perfect world, that becomes the standard and protocol.
Zac: Interesting.
Melissa: Just like, when you have a baby, they come and they check hearing and they’ve checked all the other stuff, like, we’d want to have the tongue checked as well.
I also think we could put protocols in and say what we should all do but I think maybe just the real simple of somebody when they come in and they talk, the lactations will come and I know when I had my first daughter, and they talk about why it was important to breastfeed, they definitely talked about how important it was for connection and they talked about the nutrition value but they didn’t tell me that hey, by the way, she might have some breathing issues, she might not be able to latch, she might not be able to really eat, could change the way her diet is, it could change her airway positioning.
There is some research out there now that shows that unchecked could send somebody down the road of having sleep issues. Possibly, we know that there’s a correlation in connection to ADHD with kids that snore.
I wish I would’ve gotten that information because I did not breastfeed my first daughter. I mean, I have lots of my own reasons, but I don’t know I had made my decision but I didn’t feel like I was given all the information, right. So, don’t we have the right to know everything? So, if we don’t educate the parents, how can they make an educated decision?
I don’t know so I think education is probably the first thing that would make the biggest difference.
It’s all about building these programs, implementations, having standards and I mean, listen, when I first started and it’s been like 11 years, 12 years now, and where we are today is leaps and bounds.
But as you grow new issues happening, like places like the breathe Institute, Dr. Zaghi, I mean, the whole industry change from Dr. Zaghi chose sleep, airway, tongue positioning to become his passion and his drive for research. It opened the door for so much. So, I mean, you have all these pioneers that are pushing limits and doing things all the time.
Myofunctional therapy is what you guys do, in a way, but in the mouth. So, it’s like physical therapy in the mouth. That’s really all it is.
And I feel like maybe we should also use maybe some of your standards, more to standardize what we do. So maybe I have a question for you and your fam is this. I was just like, I don’t know, anyone that ever has had a rotator cuff surgery and then they go, yeah, maybe do PT, maybe not, like I don’t know, like, it’s not an option, right?
Zac: Well, they’re doing that for total hips now but sometimes you get a total hip replacement, and they will not recommend physical therapy.
Melissa: And can I just be honest, like, is that because they have insurances? Like, where does it come from?
Zac: I’m not sure. Yeah, I don’t know.
Melissa: I am sure if we went down that rabbit hole, we could find out.
Zac: I have my suspicions. I think part of it is, you know, and in some cases, they’re not showing physical therapy as having good outcomes.
Melissa: Because it’s not quick. You got to put work into it.
Zac: Definitely.
Melissa: We have to train the tongue just like we do any muscle. You must address the structure, function, and behavior. So, fixing the structure, and not addressing how the structure got there, to me is kind of stupid. like, I don’t get it. You have to put in the work.
Zac: Yeah, and that’s the hard thing because really, any type of major lasting change has to do with a change in behavior of some kind.
Melissa: Oh, absolutely.
Zac: That is what makes our jobs that much harder as we really have to find ways to induce behavioral changes in the people, when, as humans, we inherently, if we can be lazy, we will and I don’t think that’s a fault, like a character flaw. It just, it takes work and work takes energy –
Melissa: and let’s give everybody a break. Be honest, is like what is expected of humans and for us to survive and add some kids in the mix and the house and a spouse and a dog and, you know, podcast and two jobs and or whatever it may be, to level up or do what you needed to get your hustle on or whatever, maybe there’s just not a lot of extra time.
And then you also are then to do to overcome these lifestyle changes, these behavioral changes that are going to have a Long Lasting structural and functional behavior change require self-assessment, looking in the mirror and taking time to evaluate and understand, oh, wow, I did not realize that was affecting this and connecting those dots. And when that doesn’t, so you barely have time to do these basic little exercises that we’re doing, and yet, you think you’re going to have a behavior change?
You worked with my mom. I’m going to use it as an example and my mom’s good with this because she doesn’t know what she doesn’t know. So, she came out and she pretty much just wanted to have surgery. Yeah, that was her goal. I mean, she was excited.
Now here’s me, and I’m like, you even know why you’re going to have the surgery? So, tell me exactly what’s going to change after the surgery? And I was like, No, no, you’re going to go see my buddy. And my mom is – she knows what I do for a living. She’s seen me lecture. My mother’s gotten some decent gifts of any little success I have. So, you would think she’s like, of course, I’ll go see your friend and she found out you’re out of network.
And she’s like, Oh, he’s not covered by my insurance and I was like, and that’s exactly why you are going to see him. I was going to pay for it but think about that mentality, and I’m like, Oh, my God, it’s touching nothing and then so now she comes back. She’s like, wow, how amazing. I saw her really, you know, try and working and she started to feel better. She’s like, it’s so weird. I feel better. What do you mean, it’s so weird?
I get like, so here’s somebody and I’m using this as an example. Like, it is my mother. How is she not getting and yet when something successful happens, it’s like, I wonder without, what do you mean I wonder without? She knew but it was like, she almost had to be reminded. It’s because, in her mind, the only thing that was going to fix her is if you did the surgery, or whatever it may be, right. So, if you can play on that, like not to go into her stuff, but I feel like isn’t that across the board some of the stuff we’re dealing with?
Zac: Absolutely. Well, it’s because it requires you to have some autonomy and you to have some ownership and almost intrinsic motivation to better yourself. It’s within your control.
Melissa: And most people don’t want to believe anything they’re doing or what they could do could better it because then it’s on them.
Zac: Or something that they’re doing is causing it.

Melissa: I could easily change destructive habits, but it made me struggle having empathy for people that couldn’t do that.
Where does myofunctional therapy belong?
Melissa: I think it belongs in lots of different areas: in speech therapy, dental offices, and physical therapy. I mean, it’s everywhere. I mean, it should be bodyworkers, there are so many people because it affects – it’s part of the whole thing if your mouth is weak, and your tongue is out, your mouth opened, you’re going to be mouth breathing with the oxygen is going to change, you’re not breathing through your nose, it’s going to cause sinus issues, you’re going to be more likely to have sinus stuff. It’s going to affect your face; it’s going to affect your cranial facial development, and then that can affect not that I don’t know, but neck, the shoulders, your posture.
Mom’s will be like, if so if your teeth are off like this, I was like, so how’s this constipation? And the dad’s like, well, now you fix constipation. I was like, Oh, well, I mean, if you can’t chew your swallowing whole, so hard for you know, go potty. And the mom was like “oh my god, he goes to the bathroom three times a week when that happens.” It’s really hard. I’m like, Oh, yeah, you can’t? Yes. Yes. No contact back there. He’s trying to so texture food is going to change the way he swallows the food. How quick he eats, how slow. I mean, it’s like cutting scissors that don’t line up. And he doesn’t even know to tell you. Hey, Mom, I don’t have any occlusion. I can’t chew that meat.
And we’re like, eat your food, Johnny better eat your food, close your mouth. And literally, he’s like, I can’t breathe, I can’t chew but I got to do it all so I’m just going to swallow it and real quick, get that down. It’s going to make it a lot harder for us to digest food and then digesting now sleep, right? Now that’s going to affect other things, I mean, long term and I can’t imagine that. Me talking about this, that we can’t go connect us that people that end up in your position with you are suffering from my stuff. And the people I see that are suffering from this need to be seeing you. Right? So, it’s important to keep the connection going.
Zac: Yeah, well, with that, the tongue is one component of the airway and, we’ve kind of talked about this a little bit where, you know, with you, you kind of specialize in the airway that’s more upper whereas a lot of the PT stuff that I do is more airway lower. So, you really have to, I think, blend all of that in order to elicit or to maximize respiratory capabilities, which has wide-ranging effects. You know, we talked about vagus nerve, and you look at all the influences that I have across our physiology and –
Melissa: anything when you say like your family or people I mean, that’s, that’s your place. You guys are all cool with that. So, the fact of like, your people and my people, while we haven’t all sat down had dinner, like, you know, I mean until today. That’s important because I think there’s so much, I should learn from you and you should learn from me. And I hope one day that there is a course, that helps us all connect the dots and my stuffs included in your education and your stuffs vice versa, right? Like, the idea is to up the ante and build the specialties, and really help teach the students how to connect the dots. It shouldn’t be something you have to learn once you get out of school.
Zac: Yeah. 100%.
Melissa: That should be taught in the beginning.
Zac: Yeah, it’s almost like you need a different profession that combines it all or you need a team and this is kind of where I think you are. You are realizing that you are one piece of a greater –
Melissa: Oh, yeah, I mean, I’ve known that. That’s always been but sometimes you got to do all the work to prove that you need help.
Zac: Absolutely.
Melissa: You got to show where you’re falling weak and collaboration is everything. But with collaboration, also will bring some other hurdles. Patients, like we were saying before, don’t like hard work. Well, they also don’t like being told they have to go see nine people.
Zac: Yeah, no, I and that’s an issue that I’ve ran into with some people and I think I struggle with me, referring people into this space is, when I have that conversation of well, you might need a few different things, that’s hard.
I even just look at like myself, I’ve seen, I’ve been to Lincoln, Nebraska, and then that took me to getting wisdom teeth pulled in Phoenix, Arizona, and then that took me to getting the roto rooter done in Memphis, Tennessee. And then now I’m in San Francisco getting this and then working with you and it’s just and then Zaghi cutting my tongue.
Melissa: How do you build the ultimate practice? So, the question is, does that practice look like an airway-focused dentist? and you know, this airway focus dental thing has become like, who is this person?
I mean, I hope that one day, it’s just all dentists, because it’s not about maybe others you know, they’ll be Specialists of who does what technique, but the idea of, that’s how you treatment plan. So, they actually, when you go get your six-month cleaning, it’s discussed of what your airway looks like, or, hey, if you’re mouth breathing, you can cause more decay, tell me how many of most people know that? When people are like, if you mouth breathe, your mouth is dry. If your mouth is dry, you have no saliva, you have no saliva, no antibodies, you have no antibodies, you have nothing to protect your teeth, you’re going to get more decay.

You can brush your teeth all day long. Yeah, like, where somebody else who has tons of saliva, and, you know, it goes like, so these are things like, we should always treatment plan to, hey, your tongue is not sitting where it’s supposed to, have you noticed this? And not wait till it’s to the point where now it’s like, right now you mouth breathe, you snore, you this, you have to go and drop, you know, I’ve seen my money insurance doesn’t cover. I mean, that’s a shock to the system. So hopefully that will come to a point of that. But for now, seeing groups come together and it might have a PT, it has a myofunctional therapist, it has a dentist, a body worker, but now it’s also a lactation consultant. We could go across the board.
I hope that we’ll be there and hopefully, we’ll have these great little medical many places that can offer all of that, but you got to get your group, you got to get your crew. And I feel like also as a collaborative group, you got to talk finances with each other. What are your patients looking at? What’s it going to cost for one patient to see everybody? Already, how many people know that? Like, if you refer, what’s the end of the day out of pocket? I don’t know. I’ve always been curious. I always think of that, like, so if I’m going to send the nine people. I think it’d be like, thank you for the $50,000 journey. I don’t know.
Zac: Yeah, that’s quite conservative.
Melissa: Yes, and I’ve just seen because those are uncomfortable areas, right? You don’t want to talk to your fellow colleague and be like, what you charge them. But what do you think about us working together? These are awkward conversations and I don’t know if they’re realistic. I don’t know but I feel like no one ever says it, no one ever wants to talk about it.
Zac: Yeah, but it can be a big barrier to, like, if you know so and so’s going to charge 10k for an appliance and that’s not in the cards for someone because they’re on Medicaid or something.
Melissa: It’s just not in the cards.
Zac: Yeah, you have to find a different avenue for that person to get better.
Melissa: And I mean, like, again, going back to the things like what is wrong with you? What do you do? Well, you know, money.
Zac: It’s an unfortunate thing with our system.
Melissa: Yeah, but let’s be honest, I think even in other systems, do you think they’re really addressing this?
Zac: Probably not.
Melissa: I have to say, I don’t think there’s any system that’s looking at truly getting into what’s really going on, which I’ll tell you, in all systems do. I think I could sit here and tell you that if we were more aware of some of these breathing issues, we would see a decrease in multiple things like heart issues, Alzheimer’s, I mean, we could go down the line.
It’s about more than fascia
Zac: I think all of the tissues adapt and accommodate to ensure our survival and I think if you isolate it to one specific thing, then you’re probably missing the boat. And not only that, it’s like, say you do a fascia treatment, so you mean to tell me that nothing else changed you and you were able to isolate fascia, you were able to bypass the skin? Not create a ton of changes within the muscle.
Melissa: Well, you literally had to go this whole journey to get there but nothing else was affected?
Zac: Yeah, you can’t isolate the tongue, because you’re probably going to also have influences on the teeth, the nasal airway, it all works together.
Melissa: And I think from your community and your family to ours, most people, and let’s just get medical professionals out of here, let’s just talk about our patients, the glaze people, right? You know, if you tell somebody like there’s something that’s connected to their toe all the way up to their tongue, they’re like, no, and I’m like, No, really? Because we sometimes also forget, most people have no concept of what the body actually does, or how it actually is affected. Like, really, I find that to be – they have no understanding how if I walk one way with one shoe funny for a long period of time already, that’s going to affect something.
That helps us try to explain a little bit easier to patients, how come the tongue position can affect other things? Yeah. So, learning where other systems would only make it better for us to talk about it.
Coaching breathing mechanics
Melissa: Let’s talk about breathing. We’re always hands-on, like, when you breathe, you need diaphragmatic breathing, right, like you want to breathe in. And so the beginning, we kind of tried to keep it simple for kids, it was just like a very basic of, you know, put your hands on your stomach and chest, sit up straight and don’t let your chest move. Because it’s really hard to do if you slouch.
So, it just became like, sit up straight, shoulders back, head up, because it felt like, at least opened it. But you would actually kind of had said, you know, it’s not always about sitting like that. So, what would be that something to kind of show them that we can help each other? What would be a way that you would fix that?
Zac: From my standpoint, when I look at that, you have to look at the actions that should happen at the rib cage. So, the rib cage should move as you breathe in and breathe out because if you think about it, when I take a breath of air in the tissues are filling our lungs, so the rib cage has to make room for the lungs and so it has to stand in all directions so we have these actions at the rib cage called the bucket handle, which would be lateral expansion, pump handle, which is anterior and superior expansion. And then you have posterior expansion.
But I think what you were trying to do with the belly breath is trying to mitigate an accessory muscle breathing strategy, where I’m lifting the rib cage up as a unit with muscle such as the scalene, the sternocleidomastoid. We don’t want that. I want the rib cage to stretch out.
Melissa: Yes, but you would normally want to be more about explaining how it’s rounded out and how you want to see it go like here and there. But we’re keeping and trying to be simple because oftentimes, I most of all, say like take a deep breath and it looks awful.
Zac: Well, when you demonstrated that you emphasize a lot of inhalation. Most people can’t get an effective exhale.
Melissa: Okay, yeah.
Zac: So, you have to get as much air out as humanly possible and then guess what? So, if I am just doing a belly breath, I’m not getting any expansion of the rib cage. Well, you can think of it as like my mentor, Bill Hartman, he has a toothpaste analogy. So, if I take a toothpaste tube, and I squish the top of the toothpaste tube, I get all of the toothpaste going into the bottom. Well, the same thing happens with belly breathing, when I take a breath of air in and I do not allow expansion of the rib cage, I have greater downward pressure into the abdominal contents.
So, the diaphragm will actually descend to the point where it’s flat, which creates a negative pressure environment in the thorax, which causes compression, too much outflow into the abdominal contents, which is the same thing you see in sleep apnea. But now – because what is that? I have a negative pressure environment that I can’t maintain the integrity of the upper airway, it collapses. When you’re coaching belly breathing, you’re creating the same environment, but now you’re doing it in the lower part of the airway.
Melissa: Wow.
Zac: So then now I have a mismatch of intra-thoracic and intra-abdominal pressure.
Melissa: So that is 100% correct. So, where we struggle with this is, most people I’ve noticed, I say breathe and they really do not know what the feeling is, like they really do not understand what it means to truly get a diaphragm out or like to really get that because that, like you see it in their eyes like to calm them down. So, they can’t feel that difference. So sometimes, the way we kind of were like not saying, it’s being picked from different kind of systems, and that we’ve been trained on, we got to get them to at least feel it before you can critique it.
And that the more the deeper that professionals getting, is, how do we evolve it, to also get them to feel it, but do it properly to promote positive and like, also children versus adults is going to be very different. How we do that, how we teach it, how long that habits been into play. And I am hands down. If you can’t get the breathing, right. I think miles doesn’t have a chance to stand.
So, to me, breathing has always been the biggest, has been a huge part and I have a lot of theories of like people, there are two ways that you end up with mouth breathing and one is like, there was something wrong with a structural situation with the nose early on and then that created low tongue posture because you had to breathe through your mouth. Or Yes, you had a tongue tie, right? And that tongue tie was tethered.
You could have been breastfed, but it was further back. Tongue keeps pulling down and then eventually just slowly opens and then you start to mouth breathe anyway and then you stop breathing through the nose and then that changes the way the air comes in, and now the nose becomes a face ornament, and it’s just hanging out and therefore, it’s very hard for people. They think they’re breathing through their nose, and they’re not. And you know, the ones that are like [whoo] like, though, like, you put like one of the boom, boom sticks. You’re trying to incentivize some type of nasal breathing.
When you’re stuffy, you should be doing nasal sinus rinses, 24/7 trying to force yourself to clean out your own sinus, but we go, Oh, no, I’m stuffy. Okay, you know, that’s –
Zac: It’s not normal.
Melissa: It’s not normal. You need to breathe more. I’m sick. I’m taping my lips up even more, forcing myself to breathe and it’s hard, don’t get me wrong, but you got to push through it and you will absolutely always overcome something sinus-wise; a cold or something quicker if you force more nasal breathing.
Treating adults with myofunctional therapy
Zac: Yeah. So then with your treatment process, why don’t you talk us through the – And I know it’s going to be case-specific and I hate protocols. Like that was one of my – it was a little bit of a beef with I think when you’re first learning some of this stuff is, they say, first, you do this, then you do this. You do this, do this and I think there are some case-by-case variants. Yeah. I mean, we’re doing weird stuff with me. But say someone comes to you, and we’ll say it’s an adult, because most of the family – hopefully now that you know, we’re talking about some of the stuff that.
Melissa: you’ll see with kids too
Zac: if an adult comes to you, and let’s say they have these issues, they can’t attain a palatal tongue posture, they have difficulty breathing through their nose, they have the gamut but it’s not a surgical case and maybe it’s someone that could just – they just need you.
Melissa: They just need myofunctional therapy.
Zac: They just need you. Where do you start? And maybe we could talk into your assessment and
Melissa: So, I always have to be like, well, I do myofunctional therapy very different right off the bat than most. I only do it in conjunction with dentists. I mean, almost 5% of I mean, there’s a couple of patients, I’m close with that end up knowing they’re going to go into an appliance because they’re going to somebody, but I very rarely not do that.
If I could get tongue space, probably tattooed on me. I would. For me, that’s my objective. If you don’t have enough space, I mean, anyway, if you have a lion and the little cat cage, yeah, doesn’t really matter what we do. Right. And so, I get really frustrated sometimes. I don’t know, I guess also, I don’t love to do things myself.
I mean, you’ll get changes and there’s always benefit, like even myself, if I didn’t do myofunctional therapy, I probably would have a way worse situation than I have. The therapies done quite well.
I should use myself as an example and I struggle with space, but because at least I have tongue strength, I am able to hold at least what I have so I don’t collapse so much and it’s funny a CBCT scan, if you look, my tongue is like flat up, because I have like a little cocktail straw. I have like three, four millimeters in my airway. It’s really tight. And so, I don’t have an option. My tongue can’t go back. I mean, game over, right?
Zac: Yeah, low resting tongue posture.
Melissa: Yeah. And so that’s why I can nasal breathe because I had no choice. Right? It was like, this is what it was going to be because it felt so much in my throat. So, you can do myofunctional therapy, just to be able to abstain from what you have if you don’t want to fix it, right and so, what would be the base? If someone is really good at nasal breathing, they can breathe, that’s fine and keep their lips closed and you can do an easy test like, someone just puts a popsicle stick or they hold and just breathe through their nose for two, three minutes and they’re able to do that, then yeah, I would definitely do some therapy and starting off with just doing tongue, just getting to understand where the tongue supposed to be sitting and then from there, you kind of go into being able to move the tongue and then compensation comes into play of can we separate the jaw from the tongue?
Because that’s when we really start to work the tongue muscles themselves because a lot of people think they can do things with their tongue but really, their jaws were doing it for them. And I mean, I’m no way in speech, but I always like, I asked parents all the time. I’m like, does he mumble and they’re like – we’ll say, well, do they have any speech issues? Or even adults? Oh, no, I go. Someone ever told you, you, you mumble Oh yeah, all the time. It’s kind of a speech issue. Because the mumbling is if you do not have a lot of range, you’ll notice someone will say like 123 their upper lip, like the inadequate movement of the upper lip because the lower jaw just kind of – well the tongue is down so you have to bring it up, right?
So, they reduce tone. So, they’ll talk quicker to get it out or they’ll change the words because they’re modifying. Humans are amazing. We’re going to figure it out. So those are areas that we might work in just to help you build awareness and then body scanning right? What does that feel like? Does that affect your neck? Do you feel that down in your back? Does it feel weird? Like, where do you notice it? Because if I don’t build awareness so that you feel the difference of where the tongue is? What’s going to keep you in the long run?
But I got frustrated with some cases that I wasn’t getting better. In 2017 I was pregnant and watching everything Dr. Zaghi is putting out and what’s this guy up to, whatever and I was like, oh, okay, I’m going to get this guy, I asked this guy, what about these patients? So, I actually started paying for consults for all my patients, just so I could get on this. So, I could introduce the patient, present it and ask him why they can’t go any further. I know the joke is that eventually what I was like, sorry, on staff, like, Hi, like, I was just being me and I’m presenting patient and that and now I felt like oh, my God, someone was finally able to say like, oh, the tongue, he’s tied, etc.
And now I had somewhere to send them. And I was like, ah, and now listen, the tongue tie got released and we were able to overcome it but the ones we couldn’t, which, unfortunately, were more I shouldn’t say my patients were, I was lucky enough, I already had the tool in my arsenal. There was expansion going on, right? Like I was working with doctors so if it was a BWS, which I know –
Zac: What’s a BWS?
Melissa: So BWS is a Bent Wire System, which comes from the company Myobrace and they use BWS, and then they have you wear the brace over it to kind of help do with [unsure word 1:06:10] The theory was to kind of do with the crows that did right, so. So whatever may be Crow’s out all of these different things. I was lucky enough that I had somebody that we knew we needed to make t space like that’s how we were showing that we were getting results. Or then if I would have somebody that would get good expansion, then they would relapse. That’s how long I was keeping them so that they were relapsing with me.
Because I was on this journey, I needed to know where is going. So then now, I was able to show Dr. Zaghi like, okay, we’ve done this, we’ve expanded, we’ve done, and now this has happened. And like everything happens for a reason. That’s how I was able to really so grateful for that situation. So now I was able to see, then you had that tongue-tie release in there, huh?
Zac: Because it really takes a team.
Melissa: It does. Yeah, and I know I have a hard time being like I could do the therapy, but we don’t have enough space so I don’t know. But that’s me, right? There are a lot of therapists do it. And then they only need tongue ties in there to expand and that’s fine. This is just my vehicle and that’s what I saw.
And I really do think we now finally are like getting into a community. I mean, people are talking about tongue space more and we’re more aware of the structure and that you need to be able to withhold all this, be able to have a place for the tongue, the tongue is able to be somewhere so that it can be in the right position. So, it is more and that’s what’s uneasy about it.
And then you know, they’re finally in a good place, they’ve had the release, they go home and now they have anxiety, they’re depressed, I don’t know, they get divorced, whatever their life comes into play. And we didn’t really get into the fact of what the behaviors are, and then they come creeping back, or they get a little new doggie that they’re highly allergic to, and they don’t realize it and they’re mouth breathing again.
So, the body or they’re doing you know, they have neck issues, or I don’t know all these different things, I feel like you also have to bring that aspect into it, and you have to be able to address all of it. So, the treatment planning is complex so most of the time, when a patient comes, I feel confident, I’m able to quickly say to them, okay, this is what you present with, I know your low tongue posture, you have this, this is where I would go, I would start with probably looking to get some type of an appliance. Let’s open up that bite work on that structure. While we’re doing that, let’s work on nasal breathing but while you’re getting your structure fixed, let’s work on nasal breathing. Let’s see how you feel comfortable getting your lips closed.
Seeing how that becomes comfortable and then once that structure is done the right thing, then kind of come in, let’s bring that tongue up, start noticing where the tongue spot is, and then kind of prepare for the tongue release. Because if I’m setting a patient up, I don’t want them to go get the tongue release done until they have tongue space. So then now, I’m going to focus on that, I’m going to keep it pretty structured, there was that tongue ties done. Now we go in and we do some swallowing techniques and we really kind of bring it all around, and hopefully now they’re able to keep it and now they don’t have their teeth moving and they’re not functioning as much. And if they do move a little bit, they know why they have the tools in their toolbox to go back and do the therapy again and do things on those lines,
Zac: Which again, gives them a locus of control. So then is it fair to say nasal breathing, space. Step one has to have that, range of motion, I’m assuming would be second and a little bit of awareness of the palatal tongue posture, because I would think if you don’t have the range of motion available, it’s going to be really tough to attain that position.
Melissa: Well, so right if I go back, so I don’t know for me range of motion. Okay, so it depends on so, like, we have four grades of tongue-tie, right? Then a two-step release might be the first thing to do.
Zac: Interesting.
Melissa: Yeah, just get up there. We got now we got to just do that. Then once we do that therapy, work on nasal breathing, work on the structure, then we go back and prepared for the functional frenuloplasty.
Zac: Gotcha. Because I have a client who I’m working with right now, he’s potentially a candidate for a second step. But so, they do anterior first, and then the posterior tongue tie second.
Melissa: So, the concept of why the therapy is so crucial for a tongue tie release, specifically functional for any of us, is because they need to be able to do certain exercises, certain motions and movements, and hold it during the procedure. So, they’re numb during the procedure so, they better have really good muscle memory, and know how to do these things, to hold it when you’re numb, right. So, you better be able to do a cave suction really well and also, that’s going to help build muscles. So now when the doctor goes in, and does that release, you’re going to see the separation between fascia, you know, fascia fibers muscles, it makes it a lot easier for the surgeon to get in there and see that difference.
Zac: Absolutely.
Melissa: Now anyone that’s ever worked for a doctor, anything we can do to make their jobs easier is always a win. A win for the patient, win for the doctors, win for everybody. So that’s what’s crucial for that beginning step. So, if you’re so tied, right, anteriorly, which is a lot of people that are out there that will say, Oh, I had a -you know somebody that had a tongue tie release 20 or 30 years ago, I promise you, they still need another one. Because that was a snip. They saw that it was so tongue-tied, they couldn’t move it. So, they were just doing what we do with the first step to prepare for the second one.
I mean, that’s how I look at it. Yeah, yeah. So, you know, look, I was like, Yeah, we got to give you enough rope so we can at least get you to move in, so we can get you to hit this, hit the tongue spot, and be able to then hold that cave, workup, get a little muscle tone, be able to, work there. So, we can get some identifying and be able then to get you ready for healing. And also, it’s a lot easier to do therapy exercises for healing, when you already know them and you’ve gotten muscle memory when you’re sore and in pain than it is to learn them when you’re in pain. So, I’m like, Well, why would you not do it before the procedure?
Because who wants to be learning something when they’re also sore? and it’s crucial afterward. Once the sutures off, you’re doing therapy, I mean, every four hours, six hours. You know you’ve regimented; you don’t want that stuff to reattach. You want to keep that moving. I mean, you want to use this amazing moment, and ability to – now your range of motion being so much wider, you want to continue and that’s not going to happen. You can see it become worse, tethered up if they don’t have a really great regimen and they didn’t have good muscle tone to begin with.
Zac: Yeah, and that’s something that even in PT, like, if we have someone who’s going into surgery, we try to see them – in a perfect world, you would see them pre-op for the exact same reason.
Melissa: Yeah
Zac: It makes it so much easier on the backend.
Melissa: Of course.
Zac: They have those concepts in place.
Melissa: It’s not new. And most of it all, it goes back to the implementation and trying to make sure people understand it. I think that’s going to be a battle but I think more conversations like this, more people using their mind and opening up and finding unique places to educate patients. We talk about something earlier, but not to go into I but I believe people are a little bit – I’d like to give them more credit than we do.
I think people are able to make decisions. I think we make a choice, unfortunately, to choose what information pertains to them and what they need. Because we don’t think that they have the ability to always maybe make the right decision for themselves. I don’t know. I feel like all people, this just should be spoken out. They should know, every option. Hey, if you choose not to do it once you’ve been given all the information. Okay, cool. It’s your choice. I have an issue when you weren’t presented with the side effects if you don’t do it like I’m sure if I was going and having that hip. If no one came in and told me Hey, listen, okay, you don’t you know, you couldn’t do therapy.
You could do PT prior, you know, pre and post. This is the benefits, whatever. If you don’t, you know this can happen, this can happen, this can be a little bit more challenging, not everybody, but it does happen, and you truly set the expectations and limitations of both, let the patient choose. Once they’re educated, they know, hey, do whatever you want. I have an issue that it’s not. We don’t do that.
Educating patients on airway without inducing maladaptive beliefs
Zac: Yeah, which makes sense, because then you’re not making them an informed consumer. The thing that I struggle with, and I see this a lot, and I especially see this online is sometimes when you give someone a story, and you give them the doom and gloom of what could happen, a lot of times the maladaptive beliefs that they develop from that, become an issue.
So, there was this article, this guy was named Darlow, and I forgot the name of the title is I’ll link it in the show notes. And he had this thing that this patient says basically interviewed all these patients based on what doctors had told them. Okay. And I don’t know what the doctor specifically said but the patient’s interpretation of what he said was, he was so afraid of back pain. He was so afraid of the disalignment of his back that he thought that his spinal cord was going to sever and that led to tons of anger, fear, anxiety, lack of movement, and things like that. And I especially think in this domain, because it is a huge rabbit hole and there are some scary procedures that some people may have to go down like, sure.
We’re talking about appliances and myofunctional therapy and things of that nature but what if you got someone who needs the MMA surgery? How do you balance not instilling fear and maladaptive beliefs that this is, like, if I don’t do this, my life is screwed versus informing them?
Melissa: This is what I know, I’ll just live with it. And I mean, I truly understand that. So, I said to you like I have a formula for an airway. I do this for a living. I’m aware of what I should do, right. Like, do I know that I should have surgery? It’s scary and I know, from the best. So now the other side, right? It’s human. Like, I’m going to try this first one, it’s a scary thought. And let’s be honest also I go into like, do I have it in me to do, you know, my own insecurity of will I follow through? Will, I get it done? Will it truly make a difference? And I think it’s just like, I’m always high energy. I’m always like, appear, right? My fight or flight? That’s become part of my identity. It’s who I am. Is there something inside of me that also scares me from it? Because I’m scared of who I’d be without it. I mean, I’m going a little dark here and a little deeper, but it’s, I mean, it’s my truth.
Zac: Oh, or sure.
Melissa: And I play in my own head all the time. I’m like, I can’t do it this because my kids like, you know, and I can make every excuse not to do it because at the end of the day, it’s huge and it’s a leap of faith. I think I respect that and I hope that nobody thinks that anyone’s saying it’s easy, and it’s one shot and, and do it but the question is – then the other comes back to is, maybe I just don’t think it’s affecting my life that bad. Yeah. Yeah. Even though I statistically notice.
Zac: You know what you don’t know.
Melissa: But the other thing is, you know, maybe I’m comfortable like this, I’m not ready to, I haven’t hit my place of like, I can’t do this anymore. This is no law. I can’t live like this. Right. So, I’m willing to go do that. Where I think like, in some ways, like, those are extreme cases, right? But, you know, kind of just go away. Like, let’s go to rotator cuff surgery, right, like, so that’s not something, my arms like I can’t move it, I don’t want to have a choice. That’s bottom. I got to fix it. Well, I’m almost saying like, what are we doing? Why are doctors not – Of course, PT or – Like, why would that not be automatic? I mean, that’s part of it. I feel like to say that if that’s not the standard, that’s scary. And I think things like you’ve had braces three times.
Do you want to try something different. So, you’ve had braces three times and you also have sleep apnea and so there’s a lot of things that have now are coming in your way that you’ll pay for this, this, and this. Hey, do you want to also address these other issues? Then maybe we get through there? Just those kinds of conversations.
Zac: Yeah. You have to give people options. It’s funny you when you’re mentioning the identity stuff because I totally run into some patients who will forever be a patient because that is who they are. That is their identity and that’s who they become. Yeah, you do have to wonder like if I take that away from them, so your high energy. Well, if you – you get the chill pill and I think it was in Mark Manson’s book, not the subtle art of not giving a Fuck but everything is, he talks about – I just read it the other day. Oh. In order to change who, we are, we have to mourn who we were. Yeah. It’s such a profound quote and it’s true. It’s like some people just might not be ready to go through that grieving process of changing those things, those dark things that are about you.
Melissa: Well, if you’re anxious, you’re living in the future. If you’re depressed, you’re living in the past and if you’re content you’re in the now. It’s hard. Mental health is a big deal.
Zac: In terms of like it being the X factor, or maybe the thing we’re not addressing.
Melissa: Actually, it’s personal. So, that’s like my connection to certain things. So, I had a patient, an office I was at and I walk into the room, they had the scan up. I mean, the kid has no airway. I mean, never mind, forget the cranial facial stuff and forget the teeth, who cares about the teeth? I like turned around and I was like, hey buddy, he was nervous. He’s all these things anyway. So, I was like, great. I got the assistants taken out of the room and I said so any behavioral issues like the mom starts crying. I mean, anger issues, can’t calm down, bathroom issues, can’t eat and I’m like, I want to like, just cry, right? Because I’m like, this is a kid in my mind, this young man and the mom is like, she thinks it’s just who he is, right.
Like, you know, we have one bad seed because I’m telling you, I’m telling her things and she’s like, so that has to do with that and like with a little bit of disbelief, right? Like, yeah. Right lady. No joke, the father was in there, he had a mask on, new design and I brought up one thing, I said, so is he really good in like science? And then all of a sudden, like he’s reading and comprehension seems to be lower and the mom’s like, yeah, he gets stronger grades. Then I asked if he keeps rereading the same page and the dad like takes on his thing, he goes, why he gets that from me.
Dad pulls down and he has this crazy deep bite. And I go, I know he gets it from you. I agree. You just have the same habits. And he’s like, what? I go, yeah. I go, you both, like you live in fight or flight. Like you just, I just start reading out loud. It will change the game. His dad was like, no way. So the mom’s like, I go watch it. So the kid came back and we gave him one little snippet of thing. We told him to read it to himself. I gave him three questions. and read it aloud. He was able to get it!
Zac: Essentially recruited another sensory system.
Melissa: Absolutely.
Zac: Well, and then that goes into, and I don’t know if you’ve ever checked this with those folks. Like if they have any visual issues along with that. Because a lot of times –
Melissa: I got to fix it, I’m fixing bathroom issues. Now I got to fix my eyes.
Zac: Absolutely. Yeah. Which Dr. Kareen, if you’re tuning, I got you!
Melissa: Okay. I’m sending it right. I mean, and I’m so sorry, not that I don’t know how important the visual aspect is.
Zac: Well, to me, I think this all relates to airway because if I have to assume a particular head posture, well, that’s going to change where my eyes are looking in space. And so, you could potentially see some changes in the shape of the eyes potentially, or the focusing type stuff or eye teaming.
Melissa: Well, we look at it when they, when they – Well, actually I always look like I can. They always like my little last, super what do you call it? Like my tarot card thing is I’ll walk and I’ll be like, Oh, so you only true on the left side of your face, where I looked in their mouth. And they’re like, what? I’m like, well, one side of your face is stronger than the other. I can tell you only work those muscles, but also like the moment you bring somebody up and expand them out their eyes, all of a sudden open up. because they were squinting like this.
And so, I guess, yeah, I knew the eyes were part. Everything’s affected.
Eustachian tube dysfunction
So, let’s just wrap on the one last thing. I mean, now we’ve done ears, we’ve done eyes and mouth. So, kids that have had tubes in theirs. Okay. Kids that have tubes in theirs can’t swallow, that’s why they can’t clear their eustachian tubes. So they have a swallowing issue. That’s why it keeps building up fluid.
Zac: Yeah, so wait, you’re going to have to unpack that a little bit because this is – so if someone has you stationed to dysfunction, how does that relate to the swallow? So are you saying that –
Melissa: So, normally what happens? Right. So, swallowing and I am not a hundred percent, but like if the idea of the concept of the swallowing is what helps clear it. Like it helps the fluid run through.
So, the concept of like, if you can’t swallow, so if your tongue’s low, so swallowing for anyone who doesn’t know, right. So, the tongue should be up, you should be able to swallow with minimal facial movement. The tongue should just go up, down, up very easily.
Zac: So, it kind of scoops it back. Is that how you’re approaching a swallow, it’s almost like a whip.
Melissa: but the idea is like, I drink, it’s actually suction kind of back, right. It should have like a natural sliding back to you know, kind of in a way, something along those lines, but minimal movement of the face. So, the idea is like swallowing should not be exciting to see because you shouldn’t see it, you know, something silly like that. And the truth is when that doesn’t happen and you had to work multiple swallows, like this is where chewing and right. Bulbous preparation people that have multiple swallows always have a drink while they’re eating because they need assistance when they have to swallow their food. When all that comes into play. Well, when they’re little, if there was a true issue with the way they were swallowing, it doesn’t clear everything.
So, they’re more prone to getting infections, now the tubes are in, and then the tubes came out and we had to re-put them in, and I’m sure ENTs will come back and say, well, there’s so much more to it. And absolutely, I am not giving it near all the justice it deserves.
I’m just saying, so when I’m going through and I’m looking at somebody who’s had tubes twice, they’ve had multiple ear infections. They have tonsils that are pretty enlarged, they have an elongated face, their teeth are crowded. I mean like how many things are, there’s enough there to show like there’s something bigger going on here and those are my things. My other thing is like if you had your – if your tonsils and adenoids were taken out when you were really young, I’m always like why, what created the tonsil and adenoid to be so large?
I just want to know why. I got something right. So is that maybe because they were breathing with their mouth a little bit more and the tonsils and adenoids are a secondary filtration system. It’s a backup because they didn’t nasal breathe as much as they were supposed to, so it kept the tonsils, adenoids constantly enlarge and created a lot of pressure in the back of the throat. So of course, we took them out and everything got better, but then we didn’t address the fact that they really never learned how to breathe with their nose. We just took it away and now they just continue to mouth breathe. Now they don’t even have any filter. I assume that they’re saying you have no filter in your mouth.
Zac: Interesting.
Melissa: But here I had tonsillitis like nine times.
Zac: Really?
Melissa: And I was like why? I asked my mom, why didn’t you take them out? I don’t think she wanted to tell me, but they probably did. I guess lucky for me, my mom didn’t make it to that appointment. I don’t know but I, [inaudible] I remember one summer I was in bed for like six weeks. I remember like listening to all the kids play outside and I mean, I would get, and till this day, if I’m like traveling a lot and doing things, definitely the first thing that goes, my voice will dry and I’ll get a sore throat.
I was always that kid. So, I did have those issues and I was grinding my teeth like there was no tomorrow, but I never had braces.
Zac: Wow.
Melissa: Because why? Because my tongue was plastered up there. I had to have a decent shape. Like it was right there, but I didn’t grow forward because I was keeping everything like this, so it should be out. Right. But I’m usually like what my face looked like with am I going to be able to add here was the rest of my face back, I mean [inaudible] is what you think of, right? I’m like if I’m going to have that done, I was going to have like cheek implants, I’m going to have my eyes brought out, I don’t know.
Sum up
- Clenching, grinding, and biting can be an indicator of airway problems
- Breastfeeding helps stimulate facial growth
- Mouth breathing is either caused by tongue tie or nasal restrictions
- Myofunctional therapy is physical therapy of the mouth
- Addressing upper airway restrictions requires a team-based approach
- Swallowing or lack thereof can negatively effect the eustachian tube.

