Table of Contents
Assessing and treating those who are really flexible!
Having full range of motion is a good thing, but what if you have too much mobility? Can you accurately assess someone who is hypermobile?
And most importantly:
“WAT CHU GON DO BOUT IT?”
Those clients who are hypermobile can be quite challenging in many respects. Namely, because the following is true:
- Assessments are more difficult to interpret because of increased mobility
- Coaching can be challenging
- Spotting compensations can be tough
But don’t worry, ya boi has got you covered. Here are some helpful assessments, treatment, and myth-busting when working with this population.
Check out Movement Debrief Episode 143 below to learn more!
Watch the video below for your viewing pleasure.
Or listen to my sultry voice on the podcast version:
If you want to watch these live, add me on Instagram.

 t
tShow notes
Check out Human Matrix promo video below:
Below are some testimonials for the class:
Want to sign up? Click on the following locations below:
February 20th-21st, 2021, Atlanta, GA (Early bird ends January 31st at 11:55 pm!)
April 10th-11th, 2021, Warren, OH (Early bird ends March 14th at 11:55 pm)
May 29th-30th, 2021 Boston, MA (Early bird ends April 25th at 11:55 pm!)
August 14th-15th, 2021, Ann Arbor, MI (Early bird ends July 18th at 11:55 pm!)
September 25th-26th, 2021, Wyckoff, NJ (Early bird ends August 22nd at 11:55 pm)
November 6th-7th, 2021, Charlotte, NC (Early bird ends October 3rd at 11:55 pm)
Dickinson College in Carlisle PA (POSTPONED DUE TO COVID-19) [Approved for 14 Category A CEUs for athletic trainers]
Montreal, Canada (POSTPONED DUE TO COVID-19) [6 CEUs approved for Athletic Therapists by CATA!]
Or check out this little teaser for Human Matrix home study. Best part is if you attend the live course you’ll get this bad boy for free! (Release date not known yet 🙁
Here is a signup for my newsletter to get nearly 5 hours and 50 pages of content, access to my free breathing and body mechanics course, a free acute:chronic workload calculator, basketball conditioning program, podcasts, and weekend learning goodies:
[yikes-mailchimp form=”1″ submit=”Get learning goodies and more”]
Shoulder flexion – If you need to know the biomechanics of shoulder flexion, this is the post.
Rehab Insights from Track and Field (Boo Schexnayder): This podcast will completely flip your thoughts on reconditioning and rehab upside down.
Hypermobility
Question: How do you go about assessing and treating someone that has joint laxity and hypermobility; particularly if they don’t seem to have any limitations.
Answer: Hypermobility can mean a wide variety of things to people, but let’s break this concept down to the nitty-gritty.
There are established physiological normative values for what ranges of motion our joints should be able to express (e.g. the shoulder should have 90 degrees of external rotation, the knee should have around 5 degrees of hyperextension, etc).
Range of motion beyond the established norms would be considered hypermobile.
Just as range below the established norms would be considered hypomobile.
Based on this definition, there can be a wide variety of individuals who possess hypermobility. Here are a few examples:
- A baseball pitcher with 120 degrees of shoulder external rotation
- One who can palm the floor on a toe touch
- A high Beighton Score, a hypermobility measure
- Ehlers Danlos
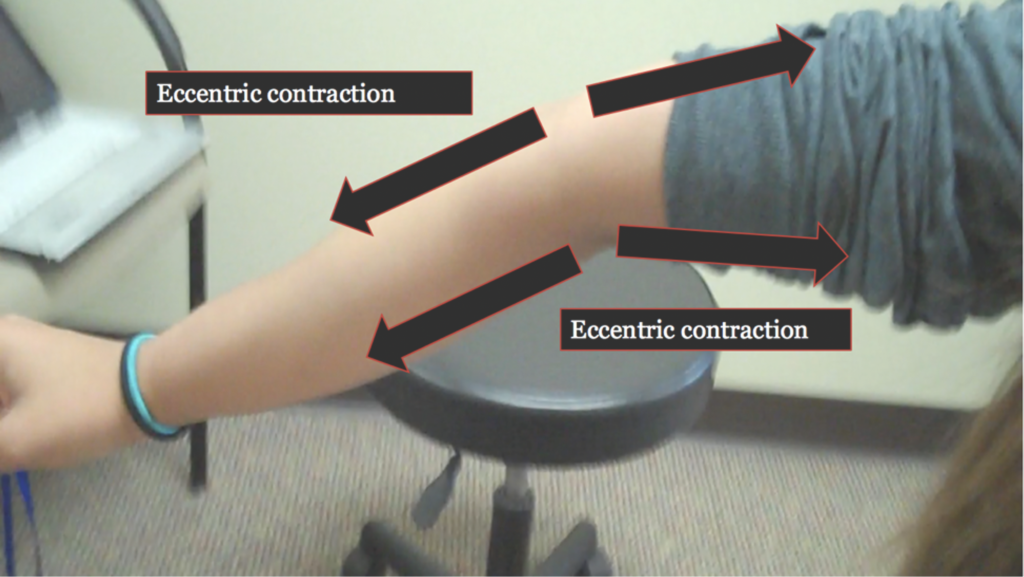
On one end, the baseball pitcher may have hypermobility in only one specific direction. On the other end, one with Ehlers Danlos has a systemic hypermobility disorder affecting multiple joints (though not necessarily all).
Although these individuals are on different ends of the spectrum, they both have similar biomechanics occurring that are creating this situation.
That is:
eccentric orientation on one or multiple parts of the joint
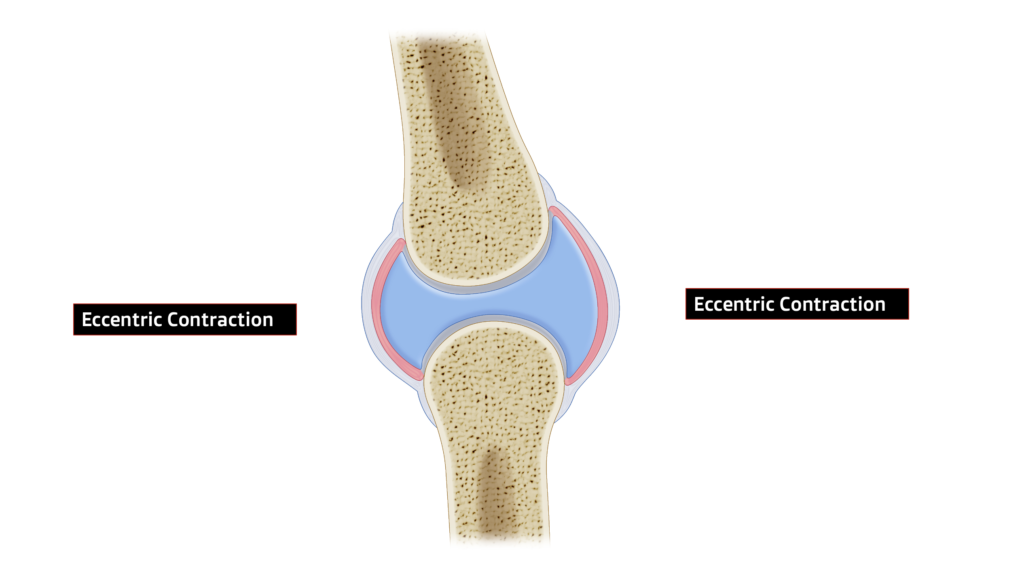
The key components of this orientation manifesting are:
- Joint space in a given area increases
- Fluid position presses up against the tissues
- ALL relevant tissues (muscles, synovium, connective tissues, ligaments, etc) increase tissue viscosity and reduce stiffness, increasing eccentric orientation and subsequent available motion.
To some extent, this process is NORMAL. The tissues in your body contain viscoelastic properties that allow them to be either stiffer (elastic, think fast folks) or less stiff (more viscous, aka flexible). Tissues have to be able to express both sides of this equation in order for movement to occur.
Hypermobility occurs when there is a loss of this process. Where the tissues develop a larger bias towards viscosity or have difficulty producing stiffness.
Now, most peeps hear hypermobility and think this is a bad thing. Hell, some people even say this is pathological.
OMG I’M PATHO AF, I BETTER JUST CALL IT QUITS
FALSE!!!!!!!!!!!!!
The problem is that there isn’t really any research stating that those who are hypermobile (except diagnosed hypermobility disorders, NOT you have a bit more hip external rotation than normal, please reread that again) are more inclined to experience pain or injury compared to those without. In fact, being able to lock out joints may have some benefits:
- Locking out joints allows for energy conservation between reps of an activity
- Locking out joints can enhance needed stability in certain phases of activity (think gait, those who lack full knee extension have worse balance compared to those with full extension)
That said, having excessive motion could potentially increase injury risk when looked at from a movement variability standpoint. People who have too many movement options cannot move joint fluids as efficiently, thus having more difficulty recovering from perturbations.
That doesn’t mean hypermobile folks are in a worse situation than stiff folks, they just may be more predisposed to other injury mechanisms. The latter population may hurt themselves from overloading specific areas due to the inability to offload structures. Each extreme can be problematic.
The solution, regardless of presentation, is as follows:
Restore all viscoelastic capabilities and contractile options
Thus, we want to first assess for any deficits, restore those deficits, then teach these individuals to generate tension.
The hard part though, fam, is that hypermobile folks may look like they move super well passively on the table. In fact, a large portion of people will lower extremity injuries have increased movement variability.
AKA YOUR APPENDICULAR MEASURES CANNOT BE TRUSTED
However, there is one area that is not predisposed to having excessive movement variability: The axial skeleton.
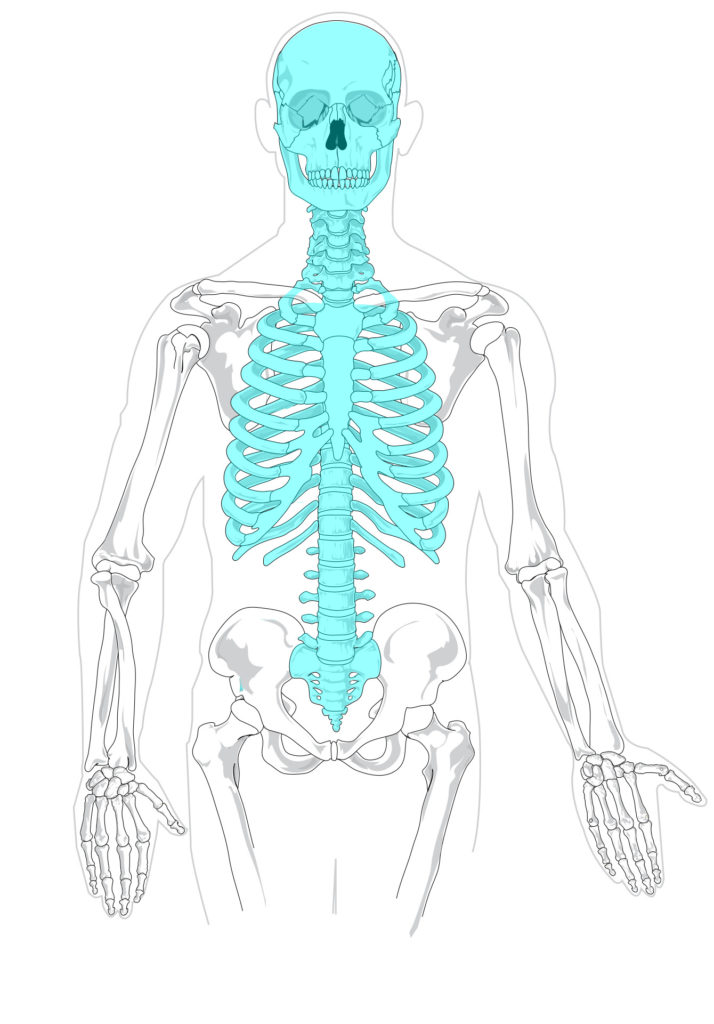
Thus, when testing these folks, you’ll want to do the following to ensure reliable testing:
- Use axial skeleton measures (Infrasternal angle, spinal rotation, etc)
- Use loaded/dynamic measures, as they may rely more on compensatory strategies when challenged
- Watch for compensations by monitoring joint motion during testing
- Appreciate end-feel, some may be actually missing the last bit of range of motion
- Note any symptoms of pain, pinching, etc, and call those points the limitation
If you pay attention, you’ll still find that these peeps present with movement limitations that need to be addressed first. many times, restoring axial movement options can positively change sensations of excessive motion.
I’ve had many clients in my day who have had what appeared to be “joint laxity” upon testing, ranging from excessive motion or even feeling aggressive/excessive joint glides as I moved them through range, that magically went away once they restored axial movement. If that’s the case, was there really joint laxity to begin with? Or was it merely a position, viscoelastic, and nervous system-influenced problem?
Once you’ve restored those movement options that were limited, you then want to focus on tasks that increase tissue stiffness.
Surprisingly, these tactics are well researched, and can be improved via the following mechanisms:
- Compression
- Long duration isometrics (20 seconds or more)
- Plyometrics
Make sure all tasks are performed with sound technique, and you’ll no doubt be a rockstar who can move well!
Sum up
- Hypermobility occurs when eccentric orientation of tissues is present, allowing for motion beyond established normal values
- Rely on axial measure testing, closely monitor appendicular measures, and use loaded/dynamic actions to see where restrictive strategies are present
- Restore movement options in limited areas first, then apply interventions geared toward increasing tissue stiffness

