Table of Contents
Keeping the upper airway open
Breathing while you sleep….it’s kind of a big deal.
So much so that things like a CPAP exist to save lives, open the airway, and get your body the oxygen it needs to survive.
But is this the best option? What happens if you have a septal deviation? Are there any measures we can take to improve airway patency while we sleep, and even train!?
To better understand what our options are, we have to look at what a CPAP actually does, and we need to have our bodies be able to do in its place if it’s something we want to cease using.
So too with nasal breathing. What are the components needed to breathe effectively through our noses?
You’ll get to find all this out today in this debrief.
Check out Movement Debrief Episode 144 to learn more!
Watch the video below for your viewing pleasure.
Or listen to my sultry voice on the podcast version:
If you want to watch these live, add me on Instagram.

 t
tShow notes
Check out Human Matrix promo video below:
Below are some testimonials for the class:
Want to sign up? Click on the following locations below:
February 20th-21st, 2021, Atlanta, GA (Early bird ends January 31st at 11:55 pm!)
April 10th-11th, 2021, Warren, OH (Early bird ends March 14th at 11:55 pm)
May 29th-30th, 2021 Boston, MA (Early bird ends April 25th at 11:55 pm!)
August 14th-15th, 2021, Ann Arbor, MI (Early bird ends July 18th at 11:55 pm!)
September 25th-26th, 2021, Wyckoff, NJ (Early bird ends August 22nd at 11:55 pm)
November 6th-7th, 2021, Charlotte, NC (Early bird ends October 3rd at 11:55 pm)
Dickinson College in Carlisle PA (POSTPONED DUE TO COVID-19) [Approved for 14 Category A CEUs for athletic trainers]
Montreal, Canada (POSTPONED DUE TO COVID-19) [6 CEUs approved for Athletic Therapists by CATA!]
Or check out this little teaser for Human Matrix home study. Best part is if you attend the live course you’ll get this bad boy for free! (Release date not known yet 🙁
Here is a signup for my newsletter to get nearly 5 hours and 50 pages of content, access to my free breathing and body mechanics course, a free acute:chronic workload calculator, basketball conditioning program, podcasts, and weekend learning goodies:
[yikes-mailchimp form=”1″ submit=”Get learning goodies and more”]
Introduction to Orofacial Myofunctional Therapy Course Review – If you want to dive into myofunctional therapy and tongue posture, this is the post for you. If you want to peep some exercises for your tongue, check out the playlist below:
Orthodontic elastics – These are great cueing devices for tongue placement
Nasal saline rinse – Clean your nostrils with this one.
CPAP
Question: My question for you has to do with the CPAP machine and why it could be bad? I know it’s a steady flow of air that can affect the pressure in the ribcage, but can you explain this further?
Would an APAP machine that does not have a constant flow of air be better? Or are there still risks?
Answer: CPAP and APAP are devices that alter the pressure of the air you breathe in, which helps prevent the airway from collapsing while you sleep.
Normally, we breathe through negative pressure. This means that as we breathe in, the diaphragm pulls downward, which creates a force that makes the airway and surrounding structures want to collapse inward. Fortunately, air getting pulled in the lungs helps maintain the shape, and life is good.
But what happens if this negative pressure is so great that the airway collapses too far and you do not get adequate airflow? Well, now you aren’t getting enough oxygen, which causes major problems. Like uh….death.
A way to “fix” this is through positive airway pressure, which essentially has the reverse effect of negative pressure—creating expansion.
Now I have a situation where I still create negative pressure from the diaphragm, but I change the pressurization of air coming into my body in a manner that allows the airway to fill. Life is good.
There are three categories of devices you could go with to utilize this mechanism:
- Continuous (CPAP): Blows a constant stream of air in under a single set of pressure
- Automatic (APAP): Samples your breathing and determines what pressure you need to be at
- Bi-level (BiPAP): The pressure changes depending on the breath cycle.
These devices are essential and life-saving for someone who has sleep apnea. This is especially true for central sleep apnea, where the brain causes the apneic events to occur. These devices can also mitigate many of the symptoms felt from sleep deprivation. So if you are someone with apnea, you most likely want to get one of these devices ASAP.
In terms of which device you choose, the BiPAP will most likely make a full respiratory cycle occur more easily, but it’s also more expensive. Your best bet is to coordinate with your sleep doc.
Now before you read onward, let me be clear:
PSA – Do not perform the following recommendations without consulting a physician first. This is not medical advice and is for entertainment purposes only.
There are a few issues with using these devices as a treatment:
- Compliance is SUPER low. 50% of users after 1 year will stop.
- Several side effects can happen such as dry throat, difficulty falling asleep, etc.
- The device may not be fixing the problem if sleep apnea is obstructive and not central.
What I mean by point number 3 is that the problem of sleep apnea has to do with the airway collapsing at some location. The machine does not fix the structural collapse but creates an artificial breathing environment; acting like a stent for your airway.
Stents open up the pipe, but don’t fix the underlying issue. This could be why CPAPs do NOT have cardioprotective effects.
You could still have many of the following issues:
- Restricted nasal airway
- Low resting tongue posture, whcih collapses the pharyngeal wall during sleep
- Low soft palate posture
- restricted airway size
- Limited cervical dynamics
- Limited thorax dynamics
All of these factors could limit your ability to breathe effectively during sleep and life. I think they need to be addressed to really “fix” the problem.
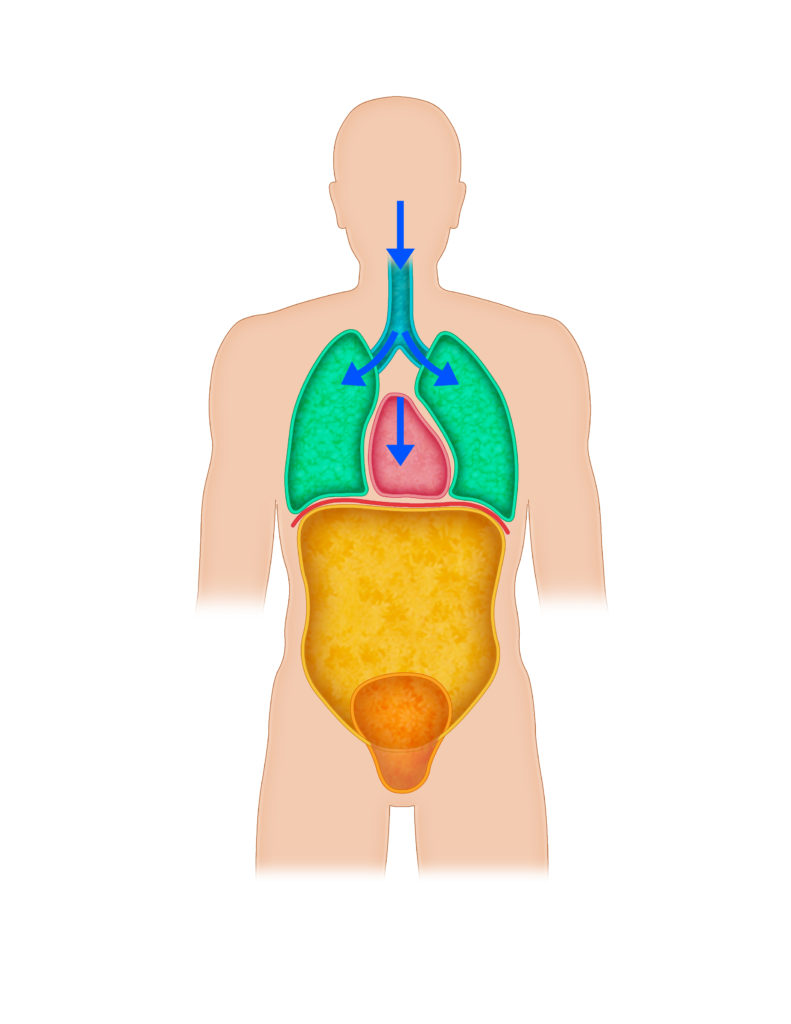
Consider if you cannot adequately breathe through your nose for whatever reason. You will not get nitric oxide production needed to dilate blood vessels, which has several cardioprotective effects by reducing blood pressure and such.
The key is to restore this mechanism.
How would you do that?
That I cannot answer, as each individual’s needs will be unique. You need data, imaging, and a physical examination to make decisions.
Pursuing upper airway restoration involves working under a skilled physician (Dentist, sleep doctor, ENT).
Treatments could include the following:
- Surgeries to impact airway at any level (maxillomandibular advancement, septoplasty or other nasal surgeries, surgical palate expansion, tongue-tie release, etc)
- Oral appliance and airway orthodontics
- Myofunctional therapy and physical therapy
- Maximizing sleep environment
- Eating foods that support a healthy sleep environment
Whatever you need, please consult a physician skilled in this domain, but I do think going this route is essential for improving upper airway dynamics, and subsequently sleep.
If you want to check out some of the stuff I’ve tried, you can see them below:
Deviated septum
Question: When dealing with a client with a deviated septum, that is a constant mouth breather. What is the best route to take with them in order for them to improve their breathing during training? Would the tongue drill help? Are there other drills?
Answer: The best route to “fix” a deviated septum would be consulting a practitioner who specializes in the upper airway.
What will likely need to happen is some changes in mouth structure and position to improve the floor of the nose (aka roof of the mouth) and potentially a surgical procedure to correct the deviation pending the degree.
There are likely no conservative measures that can alter a septal deviation, this is a structural issue.
That said, many folks can still nasal breathe well despite this structural issue. In fact, I know someone right now who has an 80% blockage in one nostril who nasal breathes like a boss!
Just like you can have osteoarthritis without pain and a high level of function, so too can you have a structural problem in your nose but still breathe well.
The key is to have all the pieces in places needed to ensure a nasal breathing environment:
- Palatal tongue posture
- Ability to breathe through your nose
- Carbon dioxide tolerance
Let’s dive into each!
Palatal tongue posture
A palatal tongue posture is the ability to place your entire tongue on the roof of your mouth and keep it there.
Notice how the tongue is right up against the roof of the mouth (photo credit: Sémhur)The ability to get into this position requires adequate mobility and knowing how to get into position.
If you want some good exercises to enhance tongue mobility, check out this post and my Youtube playlist below.
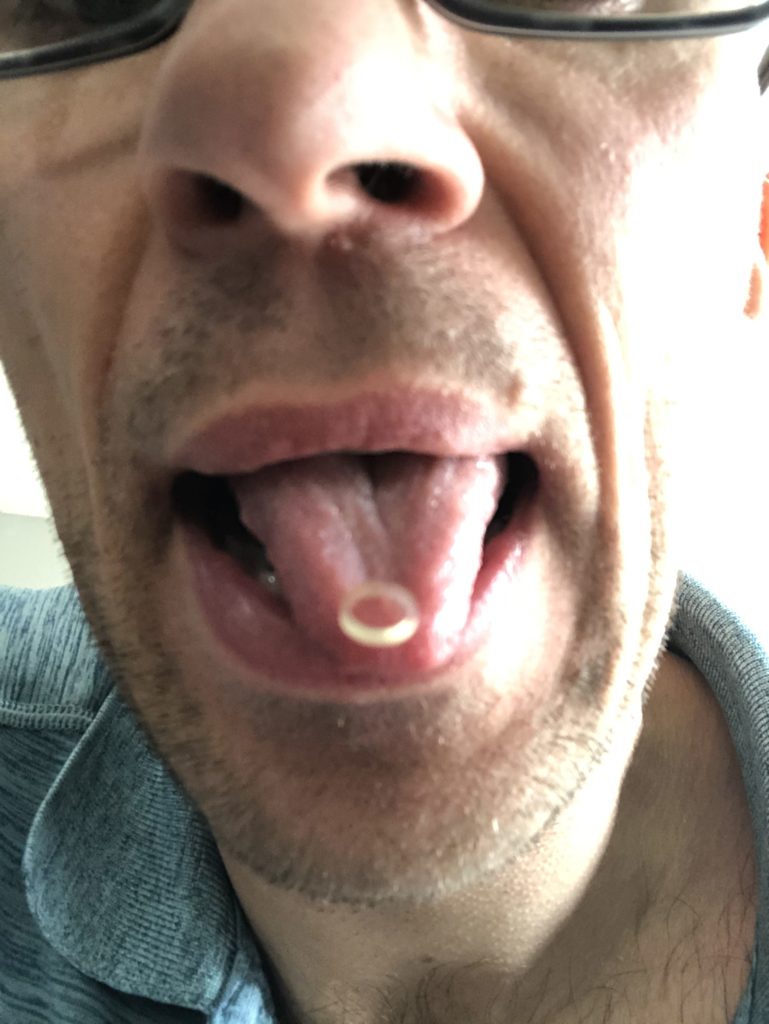
If you want to better improve tongue placement, utilizing orthodontic elastics on your mouth can be a big help. Basically, you can put the elastics where you can’t get your tongue up to as an external cue. Focus on pressing the elastic into the roof of the mouth.
Ability to breathe through your nose
This is as it sounds. Can you breathe through your nose while keeping a palatal tongue posture? Think breathe quietly and slowly through your nose in this position.
You can also use a saline rinse through your nose to keep it open and clean.

Carbon dioxide tolerance
Mouth breathing is useful for keeping blood pH in a tight window during exercise. pH is governed by carbon dioxide, so the better you can tolerate carbon dioxide, the longer you can nasal breathe.
This quality can be improved by working on a controlled pause. Here are the steps to this action:
- Attain palatal tongue posture
- Exhale a normal amount through your nose
- Pause and do not breathe. Hold to the point of first experiencing air hunger (where you feel the need to breathe in)
- Breathe in lightly through your nose, and exhale again; repeating step 3.
Over time, your ability to tolerate air hunger should improve, and NO ONE will mess with you.
Sum up
- CPAPs help keep the airway open and oxygen in your body, but improving airway dynamics and structure are key to “fixing” sleep apnea
- Nasal breathing requires a palatal tongue posture, regular nasal breathing, and carbon dioxide tolerance
Image by https://www.myupchar.com/en