Category: All Things Rehab
3 Exercises That Fix 90% of Low Back Pain
Discover three transformative movements to alleviate lower back pain, enhance mobility, and improve overall comfort with our expert guide. Say…
Fix Upper Back Tightness FOR GOOD
Discover effective strategies to alleviate upper back tightness for good. Learn biomechanically sound exercises that expand ribcage space, mobilize the…
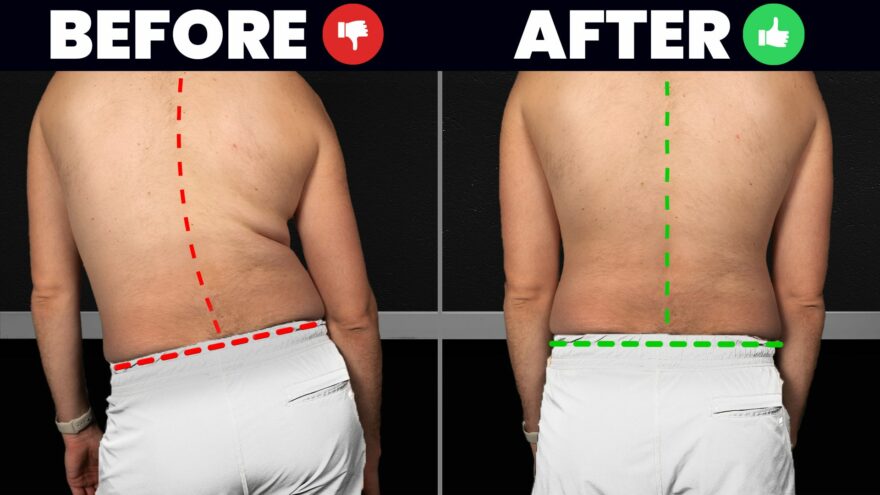
Fix Lateral Pelvic Tilt FOR GOOD
Discover effective strategies to correct lateral pelvic tilt and improve hip mobility. Learn targeted exercises for a balanced posture and…

Fix Hip External Rotation (FAST)
Discover the top 3 strategies to rapidly improve your hip external rotation in 2024. Learn biomechanically sound exercises that enhance…

Do These 3 Exercises to Start 2024
Kickstart your 2024 with these 3 groundbreaking mobility exercises! Discover how to enhance your movement, improve rotational mobility, and feel…

Ignoring These 5 Mistakes Will WRECK Your Mobility
Revamp your mobility routine in 2024 with these crucial tips! Discover the top 5 things to stop doing for better…
3 Exercises That Fix 90% of Elbow Pain
Discover the top three exercises to alleviate 90% of elbow pain. Learn simple, effective techniques to improve elbow mobility and…

Bulletproof Your Knees
iscover the ultimate guide to bulletproof your knees. Learn effective exercises and techniques to enhance knee health, mobility, and strength…

Foam Rolling is Making a Comeback? (Not How You Think)
Discover innovative foam rolling techniques for enhanced mobility and muscle soreness relief. Learn about exercises that go beyond traditional methods…

Fixing Your Knee Caving for GOOD
Unlock the secrets of knee valgus with our in-depth guide. Learn why your knees cave in and discover exercises to…

5 Ways to DESTROY Your Mobility
Discover the five common mistakes that can ruin your mobility and learn how to fix them for better range of…
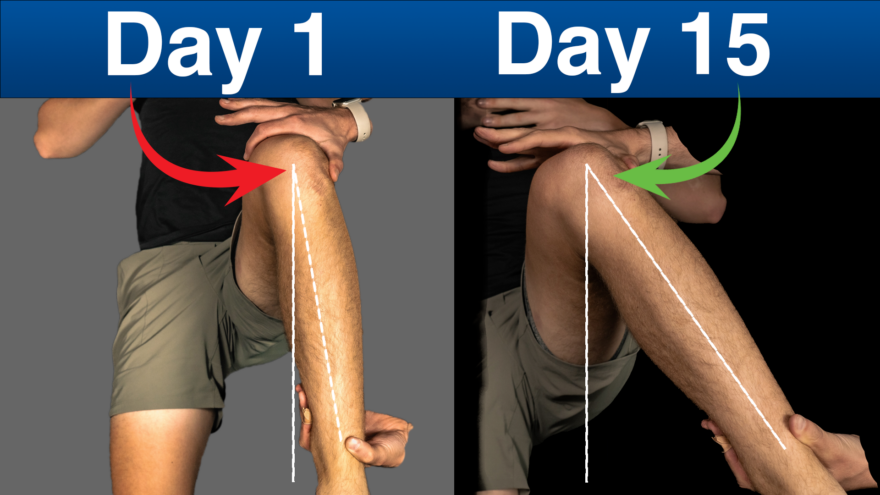
Upgrade Your Hip Mobility (FAST)
Unlock the secret to better hip mobility with our ultimate guide to hip internal rotation. Learn the biomechanics behind this…
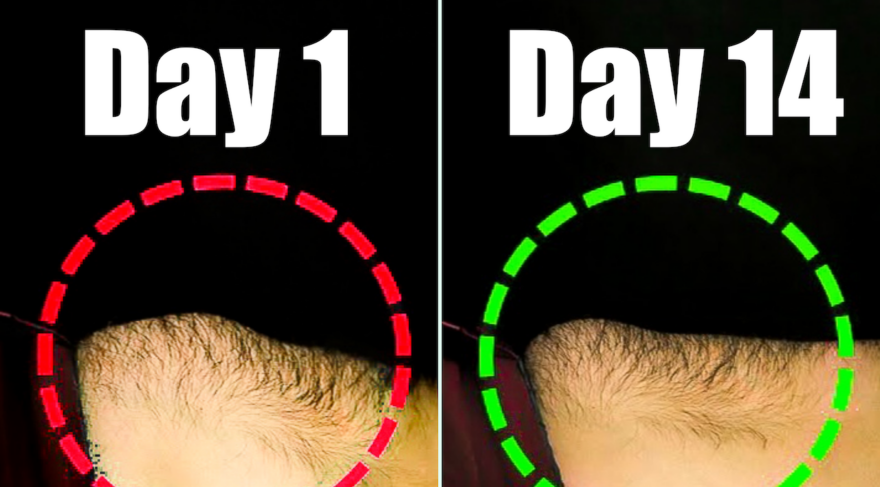
No More Protruding Pooch Belly in 2 Weeks
Ever wondered why your lower belly sticks out, despite all the crunches? Uncover the secret cause of pooch belly that…
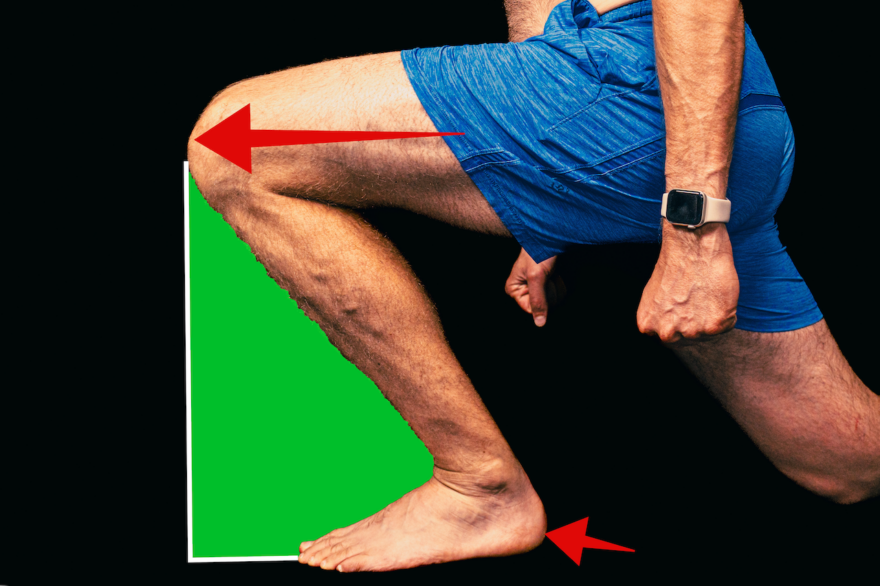
The Hidden Key for Ankle Mobility
Unlock the hidden keys to ankle mobility with this comprehensive guide. Dive into the intricacies of foot and ankle motion,…

I Stopped Doing This Exercise FOR GOOD
ver tried the 90-90 exercise and wondered if there’s a better way to improve your mobility? ? Well, you’re in…
