Category: All Things Rehab

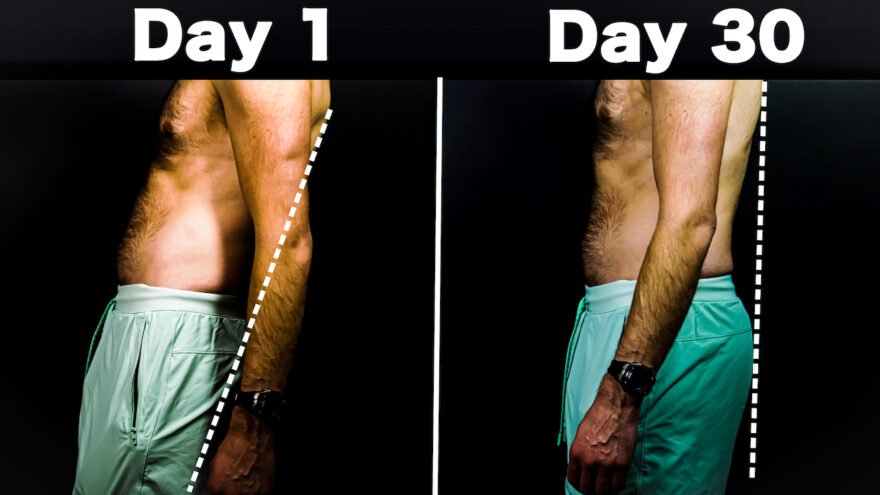
Everything Wrong with Bryan Johnson’s $2M Posture Routine
Bryan Johnson: A Man of Many Talents, but is Posture Advice One of Them? You’ve heard of Brian Johnson, right?…
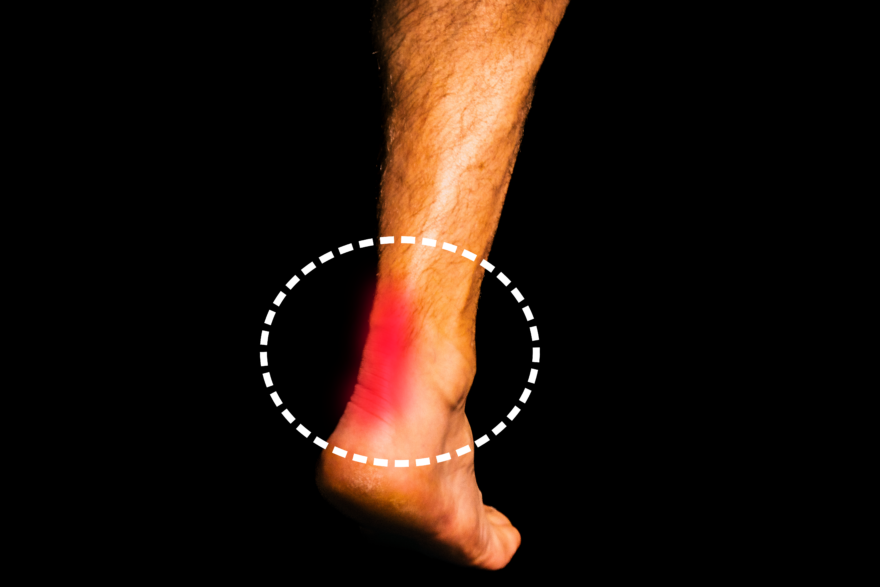
I Beat Achilles Tendon Pain FAST (Instant Relief)
Learn how to manage Achilles tendon pain with a four-step approach involving load management, improving movement dynamics, nutrition, and local…

You’re Missing This When You Walk
Make Walking Comfortable I want you to think back on your last leisurely stroll or intense power walk. Did you…
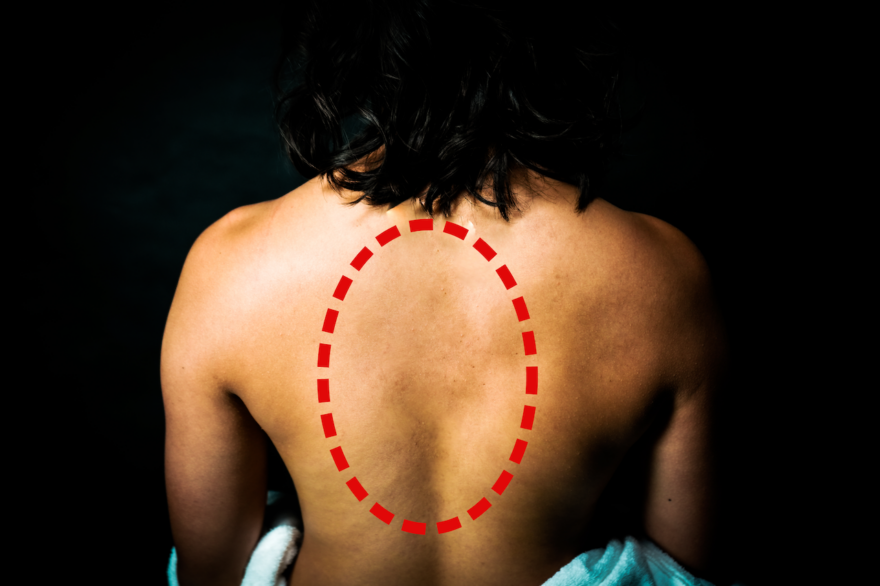
Something’s Up with Your Back…
A common postural problem Slouched posture gets all the press, but what if you’re dealing with flat back posture? Although…
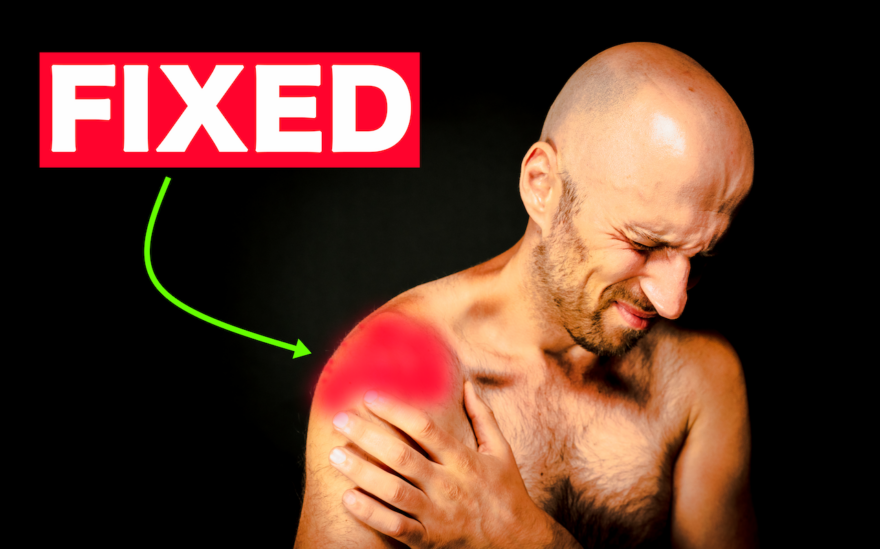
4 Exercises That Fix 90% of Shoulder Pain
That NO ONE looks at Almost all painful shoulders neglect improving mobility in 1 key area. An area that services…
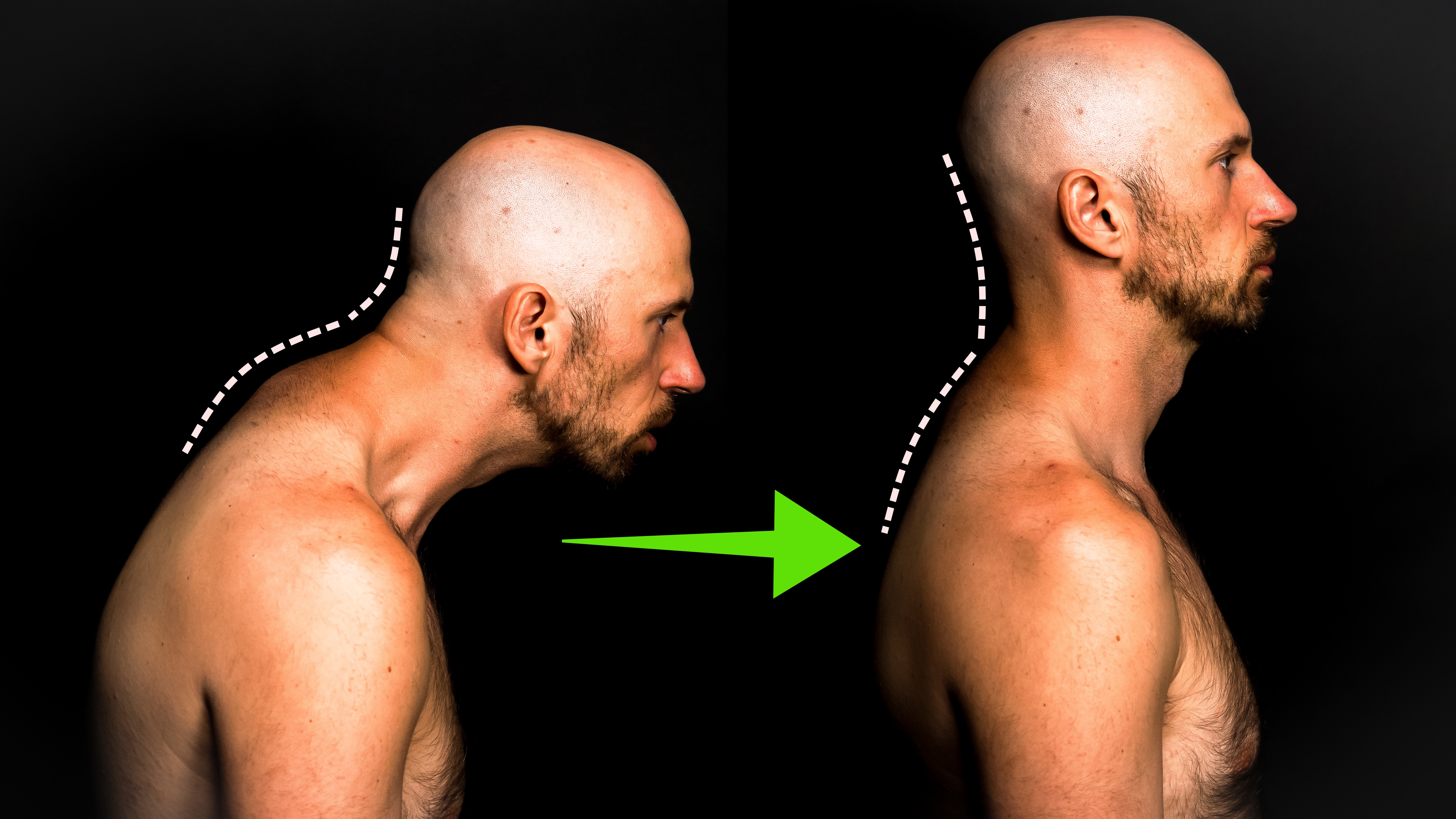
Fix Forward Head Posture for Good
Addressing all factors that cause forward head Struggle with forward head posture? I bet you tried sitting up straight and…

The WORST Thing You Can Do for Tight Hamstrings
A better solution for tight hamstrings If you often feel that your hamstrings are tight, your first thought might be…
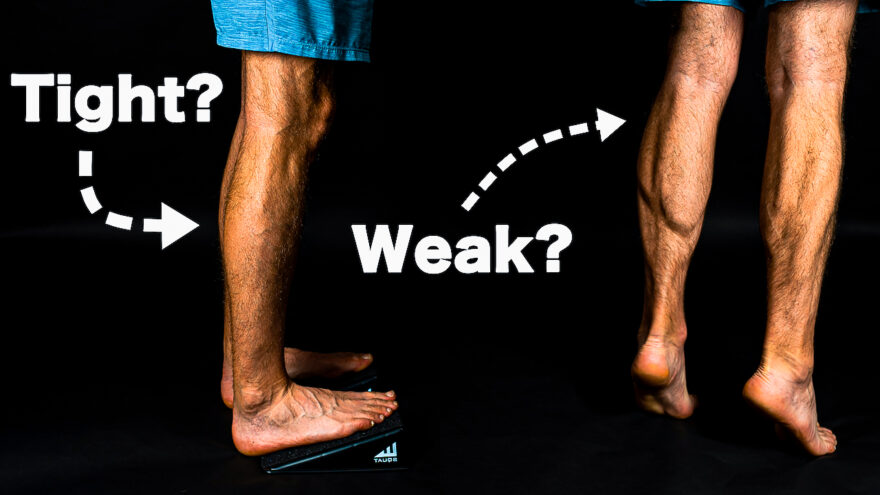
99% of Leg Exercises are Missing This
Nailing this one thing changes lower body exercises forever Spending hours doing mobility drills to get loose, but not seeing…
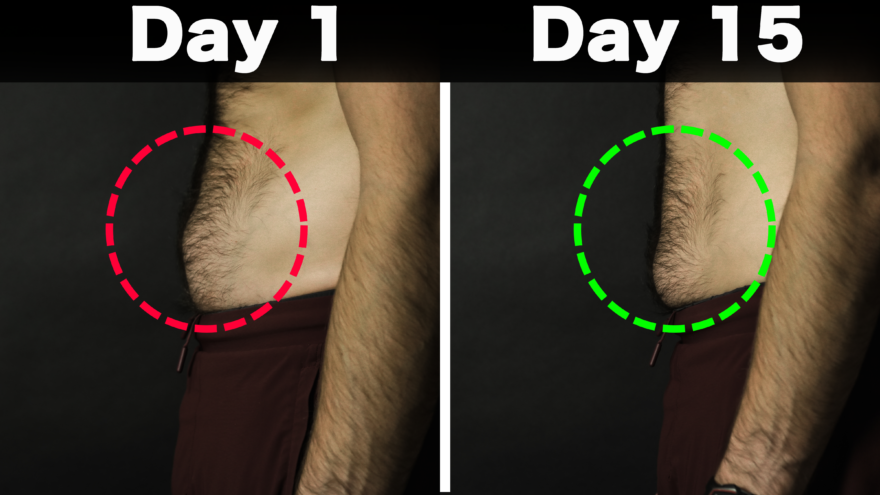
FIX Belly Pooch for Good
The cause No-one Talks About It can be frustrating to work hard to lose abdominal fat, only to be left…
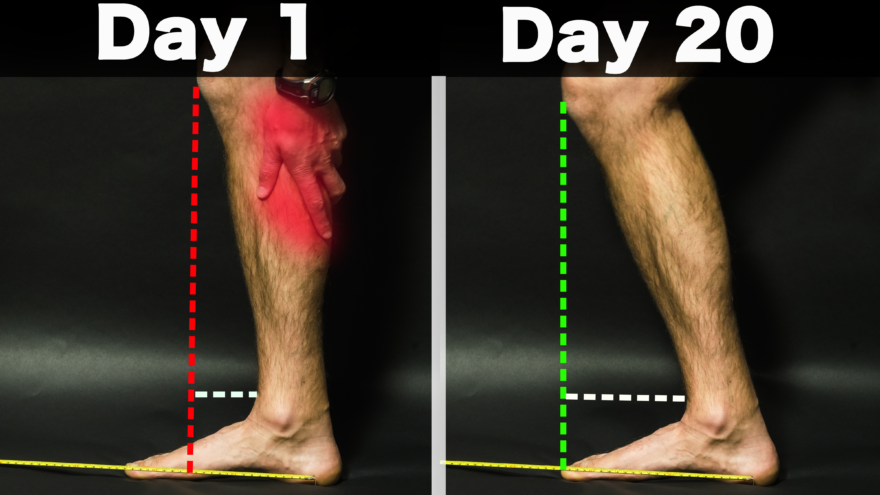
The Only Thing You Need to Fix Tight Calves
The real reason your calves are always tight Are you tired of feeling like you’re walking around with bricks attached…
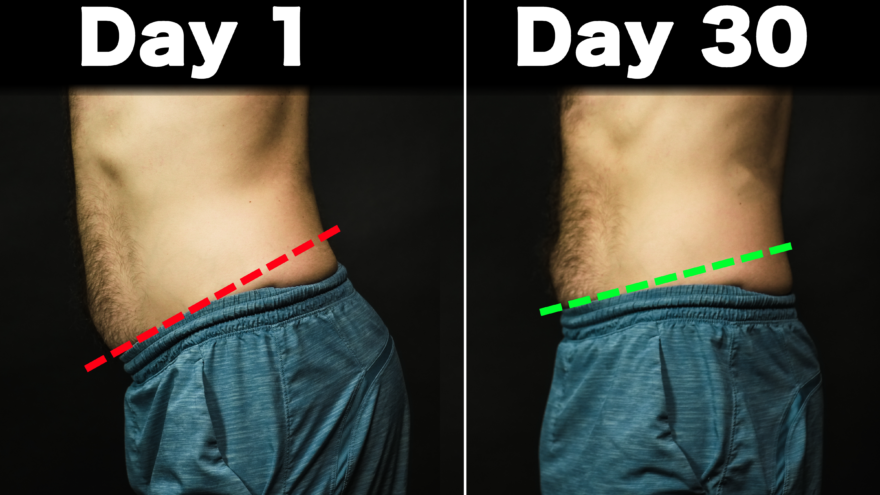
Anterior Pelvic Tilt – Fix it for Good
Is anterior pelvic tilt something I NEED to fix? If you’ve ever thought you have an anterior pelvic tilt, you’ve…

3 Exercises That Fix 90% of Problems
THIS is why you’re so darn stiff Ever wake up feeling like a stiff robot (not the cool dancing kind)?…

The Overpronation Hoax (and the truth)
You MUST pronate, here’s why Think you’re a victim of overpronation – the evil villain in the world of foot…