Tag: physical therapy

Fix 90% of Pelvic Tilts in 30 Days
Enhance your hip and pelvic mobility with our comprehensive guide, featuring detailed testing and exercises developed over 13 years as…
The Last Pelvis Post You’ll Ever Need
Unlock the secrets of pelvic biomechanics to enhance mobility across your lower back, hips, and legs. Master movements that mimic…

5 Exercises That Heal the Body
Discover how to alleviate pain and improve mobility with these five tension-reducing exercises. Perfect for enhancing movement fluidity and reducing…
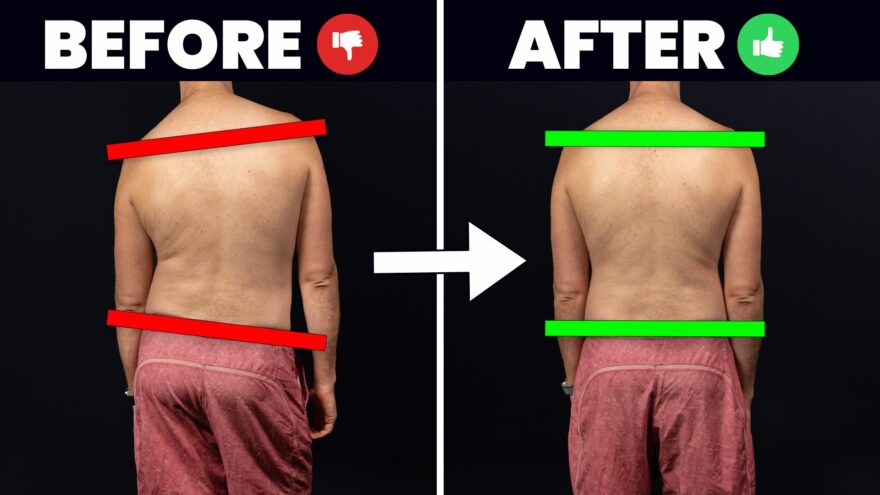
Fix Posture and Muscle Imbalances FAST
Discover the ultimate guide to correcting posture and muscle imbalances quickly. Learn how to measure your body’s unique asymmetries and…
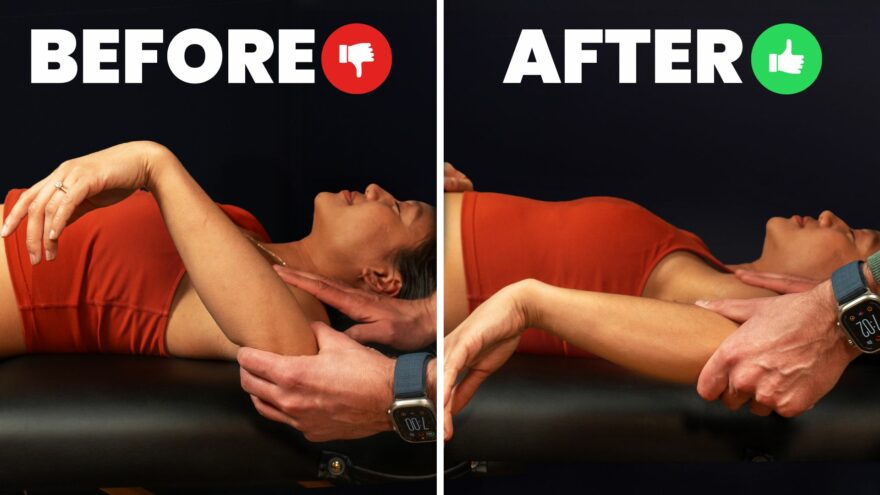
Fix Your Shoulder Internal Rotation FAST
Meta Description: Unleash your shoulder’s full potential! Discover simple yet effective exercises to rapidly improve shoulder internal rotation, enhancing your…

Ignoring These 5 Mistakes Will WRECK Your Mobility
Revamp your mobility routine in 2024 with these crucial tips! Discover the top 5 things to stop doing for better…

Top 5 Mobility Drills of 2023
Discover 5 revolutionary exercises to boost your mobility and performance, as featured on our popular exercise channel. Perfect for overcoming…

Foam Rolling is Making a Comeback? (Not How You Think)
Discover innovative foam rolling techniques for enhanced mobility and muscle soreness relief. Learn about exercises that go beyond traditional methods…

The Hidden Cause of Scapular Winging (That Experts Miss)
Ever felt like your shoulder blade’s trying to take flight? It’s not just about the muscles—it’s the stage they perform…
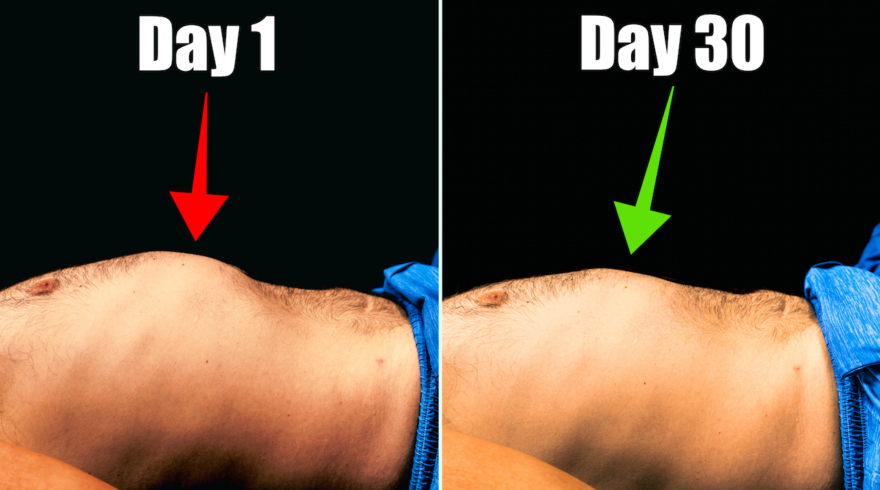
Fix Rib Flare Once and For All | 30-Day Challenge
Rocking a rib flare that’s cramping your style? Discover a sequence of exercises that can reshape your ribcage and get…
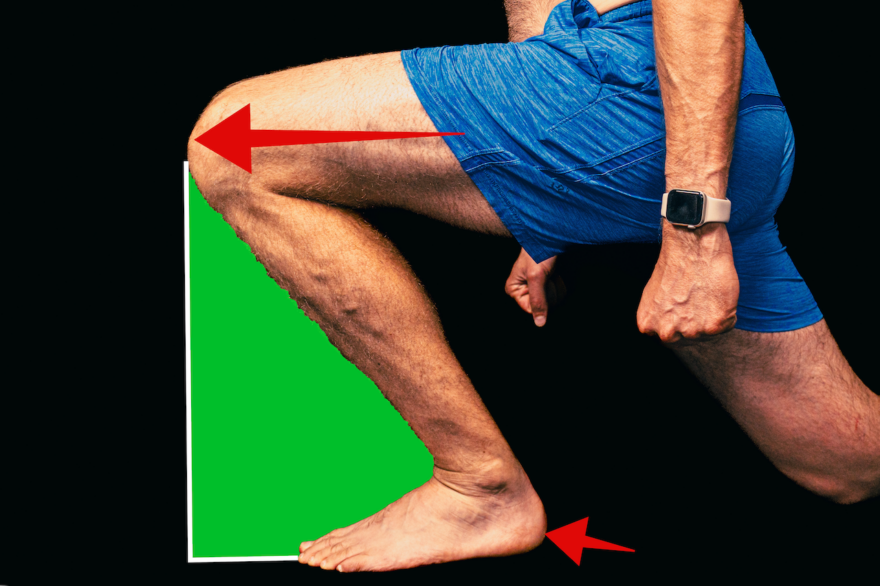
The Hidden Key for Ankle Mobility
Unlock the hidden keys to ankle mobility with this comprehensive guide. Dive into the intricacies of foot and ankle motion,…
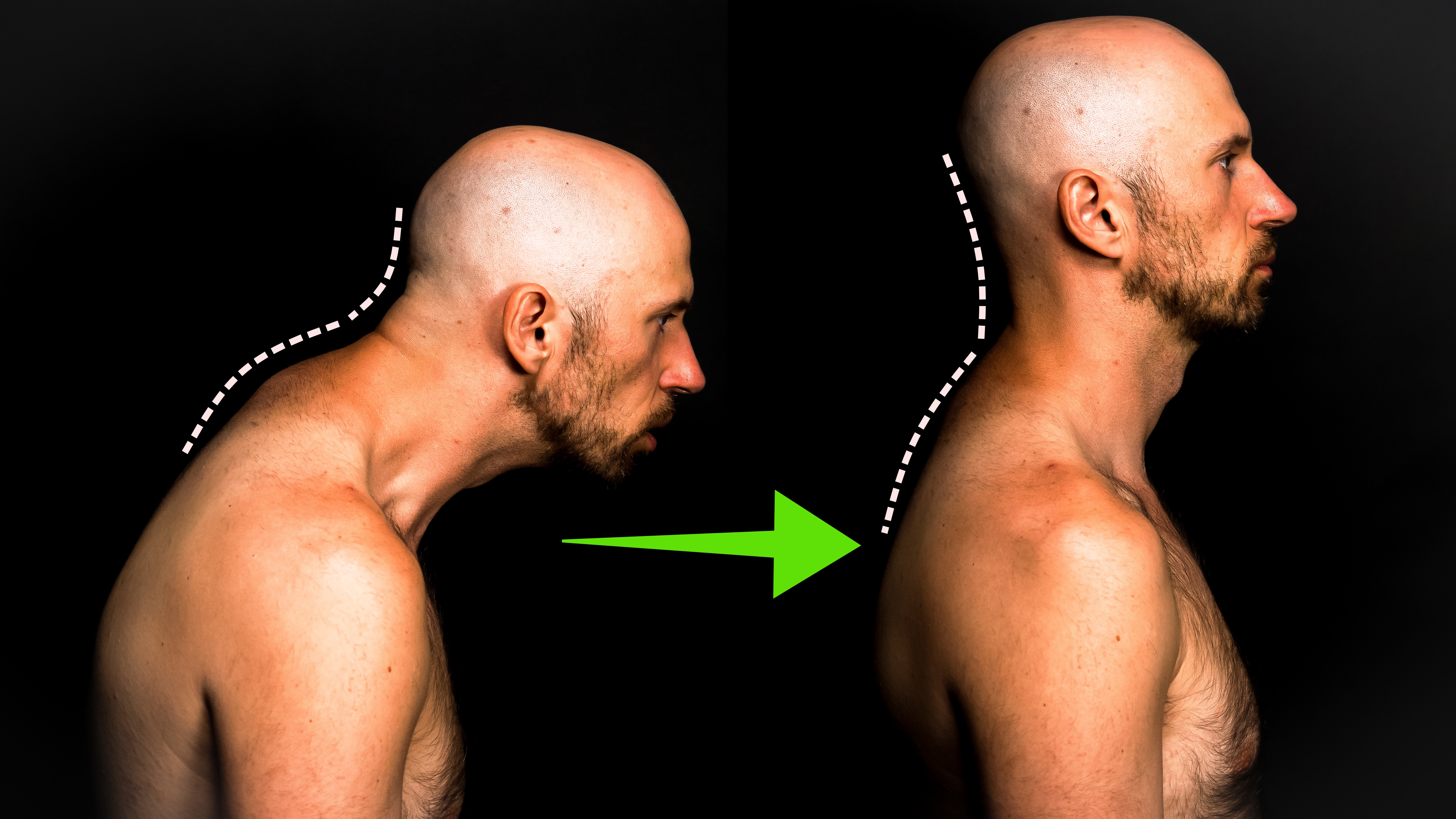
Fix Forward Head Posture for Good
Addressing all factors that cause forward head Struggle with forward head posture? I bet you tried sitting up straight and…
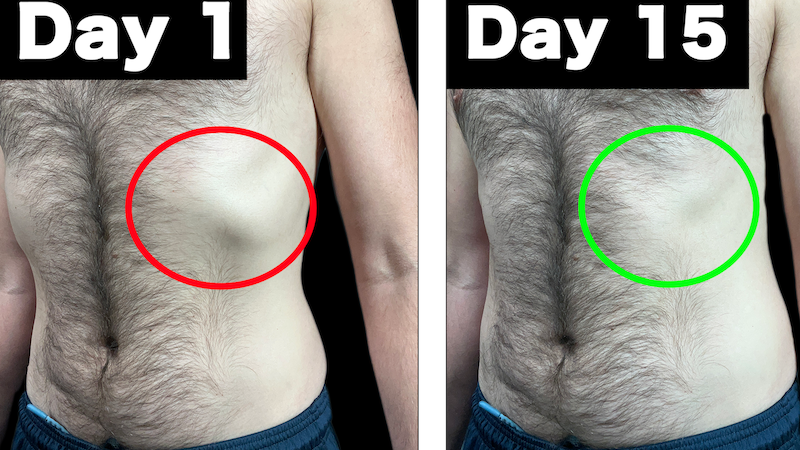
The BEST Rib Flare Fixing Exercise
This move fixes it for good! Are you tired of living with a rib flare? Do you want to improve…


