Tag: breathing
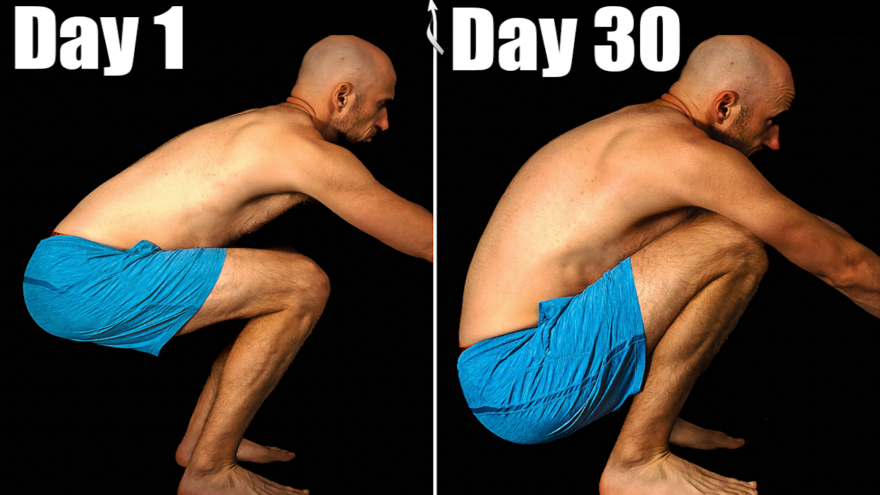
Fix Everything in 30 Days
Feeling stiff and achy all over? Before you dive into a complex 10-step program for each pain point, let’s simplify.…

Don’t Ever Breathe This Way
You’ll RUIN all the benefits Breathing exercises can reduce stress and anxiety, but their effect sizes are small. Nor have…

The Pot Belly Cause NO ONE is Talking About
What if the pot belly wasn’t only belly fat? So belly fat, gut issues, and pathology can definitely create a…

The Best Free Course to Learn Advanced Biomechanics
Struggling with all the confusing breathing stuff on the internet? Learning biomechanics can be so tough because EVERYONE uses confusing…
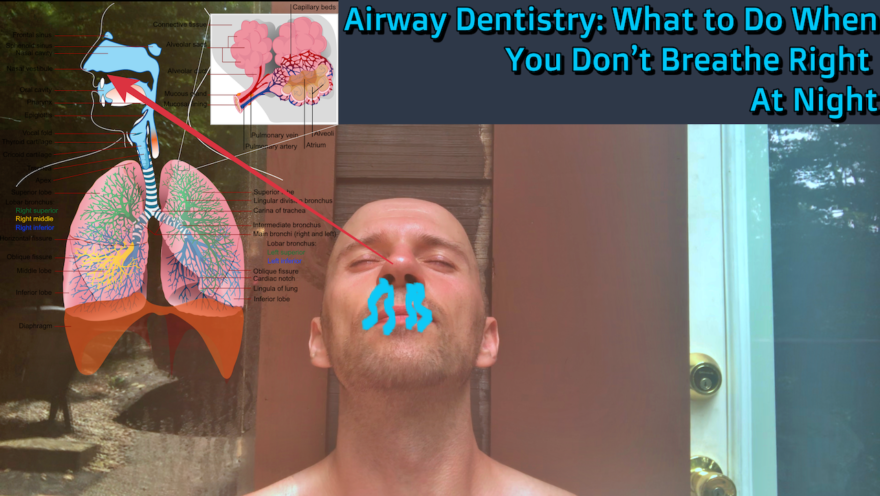
Airway Dentistry: What to Do When You Don’t Breathe Right At Night
If you are having trouble sleeping, snore at night, or mouth breathe like none other, you definitely have to listen…

Improving Hip and Shoulder Internal Rotation WITHOUT STRETCHING!
Having shoulder and hip internal rotation is kind of a big deal. What if you could get it as quickly…
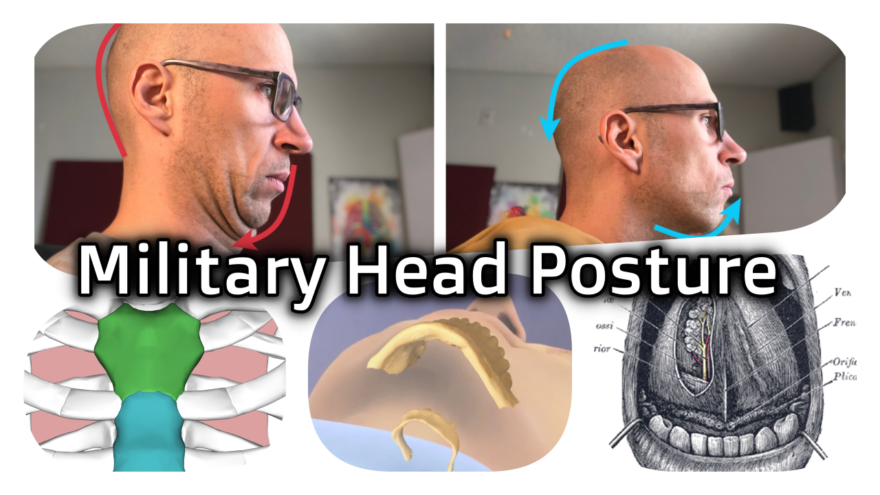
Military Head Posture
If you have a military head posture, double chins, and aren’t sleeping like a boss, you mos def gotta check…

The Evolution of My Treatment Process
What has changed in my treatment model? If you aren’t getting better, you are getting worse, so how has your…

Mindful Movement with Lucy Hendricks
The trainer’s guide to teaching clients the fundamentals of health What does it take to make clients healthy? Is it…

Top 10 Posts of 2020
From upper airway to infrasternal angles, some of the best posts to consume on my site are right here!

How Breathing Impacts the Human Body
If you want an intro to all things breathing, it’s effects on your mobility and physiology, this is a great…

Manual Therapy
Does manual therapy have a place? Manual therapy is one of the more polarizing topics in the movement world, and…

Incorporating Breathing into Training
Struggle knowing where breathwork fits? You might be head over heels for all things breathing, but what if your clients…
Which Limitations to Treat First?
So you have all these limitations you’ve found. You may inevitably ask yourself: Uhh…where do I start, fam!?!? This post…

