The hand has always been a weak area of mine, anatomy, treatment, the whole 9 yards. Thus, I was inspired to take an Intro to Hand Therapy Class taught by Patricia Roholt, a certified hand therapist (CHT) with 30+ years of experience.
The intent of this class was to provide a broad overview of all things hand therapy. We dove into hand anatomy, evaluation, treatment, splinting, and specific conditions.
My favorites parts were the anatomy, evaluation, and splinting sections. All of these areas were weak points of mine, and I definitely achieved quite a bit of clarity with these concepts. P-Ro is an absolute monster when it comes to splint making, and I loved all the tricks up her sleeve she had to make effective splints. It’s an area I’d like to dive into a bit more.
if the above areas are what you consider to be a hole in your game, I’d consider checking out her online offerings to see if her courses would be right for you.
Check out the full review in the video below. Once you got my final verdict, check out some of the meaningful highlights in the notes below.
Table of Contents
Hand Anatomy
Let’s look at some of the fascinating anatomy that accompanies the hand.
The Carpal Bones
Laying your anatomy foundation starts with carpal bone appreciation, and the potential accompanying clinical problems.
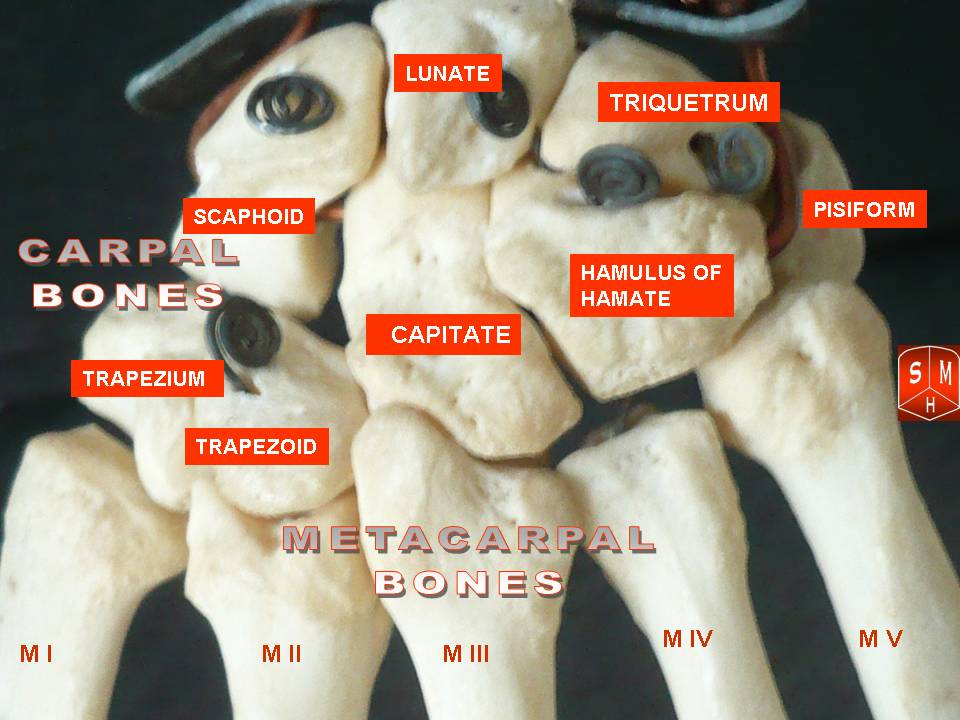
As you can see, there are two rows of carpals. In the proximal row, the scaphoid and lunate articulate with the radius, and the lunate and triquetrum articulate with the ulna. The pisiform is in this row as well, but doesn’t articulate with any other bones. Its function is to allow for passing of the ulnar nerve and artery, and provide a distal attachment for the flexor carpi ulnaris (FCU).
The big red clinical red flag that can occur in this row is a scaphoid fracture. Because of poor blood supply to this bone, people often needed to be casted for 2-4 months to allow for healing.
Fractures in this region are often not immediately visible on imaging. Thus, a subsequent x-ray ought to be performed 2-3 weeks after the initial injury.
The second row of carpal bones consists of the trapezium, trapezoid, capitate, and hamate.
The trapezium is a bone of interest. In individuals undergoing surgery for thumb carpometacarpal joint (CMCJ) arthritis, part or all of this bone is often removed to increase space. Space is further increased by harvesting the palmaris longus tendon and shaping it into a pseudo-trapezium.
The Hand’s Retinacular System
The retinacular system ensures that tendons stay adhered to the hand while gliding, allowing for optimal hand function.
We can break up the retinacular system into three areas:
- Extensor retinaculum – made up of six compartments (with first compartment potentially contributing to DeQuervains tenosynovitis)
- Flexor retinaculum – Contain several synovial sheaths. Fingers II-IV all have their own sheath, whereas fingers I & V share a sheath.
- Finger retinaculum
The most complex of these systems is the finger retinaculum. There are several pulleys that compose this system to adhere the flexor tendons to the finger: five annular pulleys (A1-A5) and three cruciate bands.
These pulleys are arranged in the following sequence:
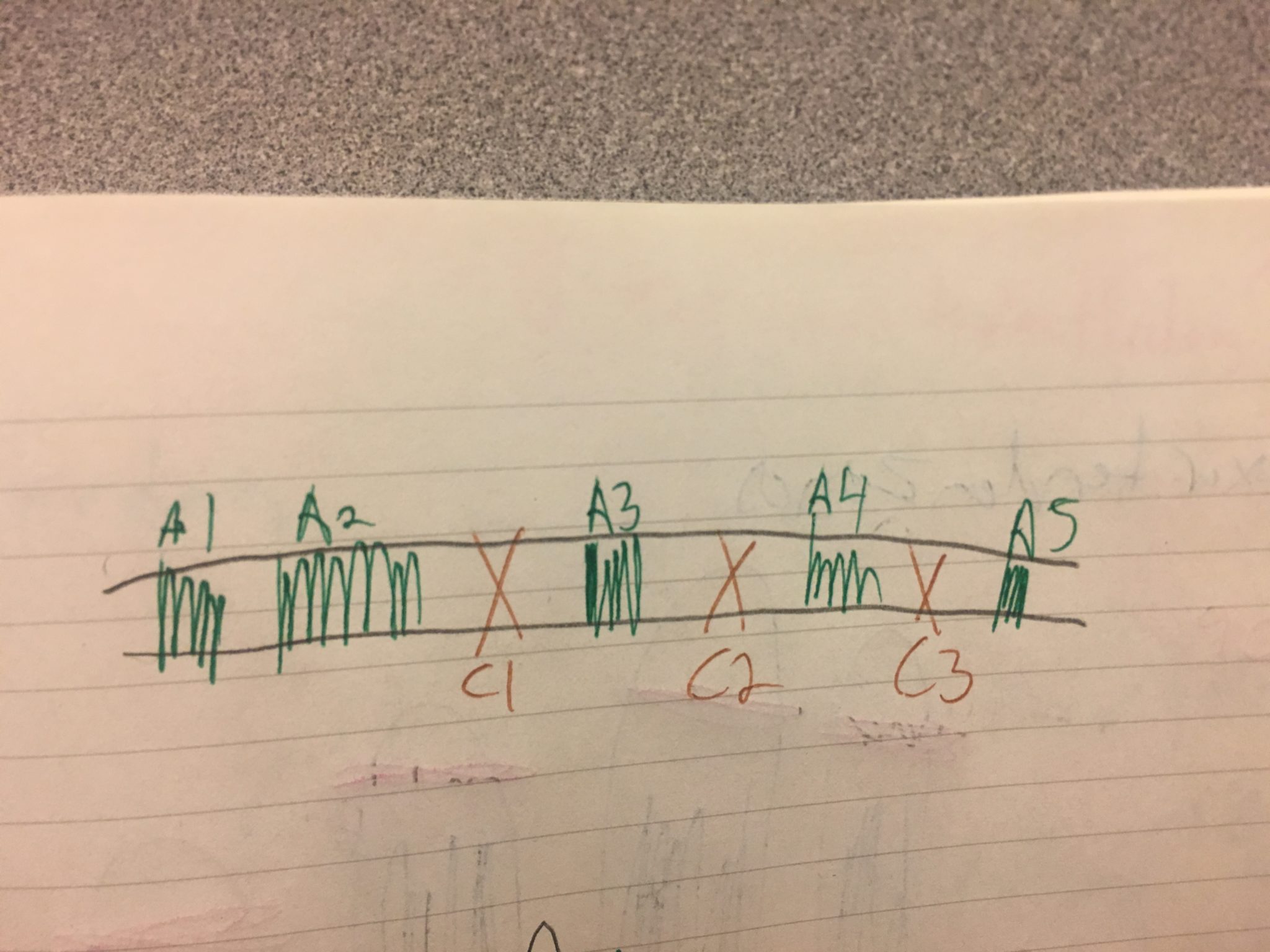
For reference, here are the location of the Annular pulleys:
- A1 – Metacarpophalangeal Joint (MCPJ)
- A2 – Half the length along the proximal phalanx
- A3 –Proximal interphalangeal joint (PIPJ)
- A4 – Middle phalanx
- A5 – Distal interphalangeal joint (DIPJ)
Trigger finger is a condition implicated within this system. Inflammation and swelling can adhere flexor tendons to the A1 pulley, restricting finger extension. Surgically, the A1 pulley is cut to alleviate this condition.
The Zones of the Hand
There are five zones of the hand to describe portions of the volar surface. It is important to know these zones from a surgical standpoint.
 Pink = zone 1; black = zone 2; purple = zone 3; green = zone 4; blue = zone 5
Pink = zone 1; black = zone 2; purple = zone 3; green = zone 4; blue = zone 5
- Zone 1 – Proximal to Flexor digitorum profundus (FDP) insertion
- Zone 2 – From Zone 1 to A1 (considered no man’s land due to poorest recovery times, as hand intrinsics reside here)
- Zone 3 – From A1 pulley to volar carpal ligament
- Zone 4 – Carpal tunnel
- Zone 5 – Proximal to carpal tunnel up through forearm
Keeping flexor tendons healthy post-surgery involves differentially gliding their tendons. These movements help prevent flexor tendons adhering to the pulleys.
To understanding how to effectively perform these maneuvers, we need to understand flexor tendon muscles.
The big two that we are differentiating are flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP).
FDS primarily flexes the PIPJ…

…while FDP flexes the DIPJ.
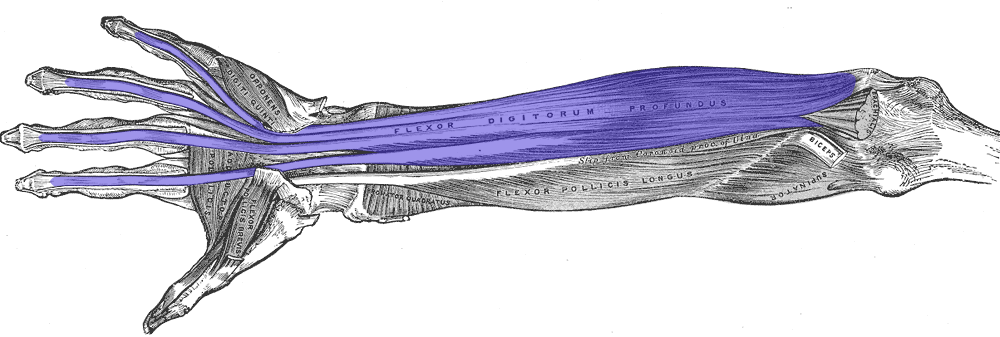
Thus, maneuvers must be performed to ensure individual gliding:
It is also important to note that FDP has two separate muscle bellies: one that goes to finger II, and the other that is shared by III-V. Thus, injuries along these particular areas require protection of all fingers, and may require joint blocking exercises to ensure tendon health.
The Extensor Mechanism
Whew, this part is a beast and very complicated structure. Let’s see if we can sift our way through it.
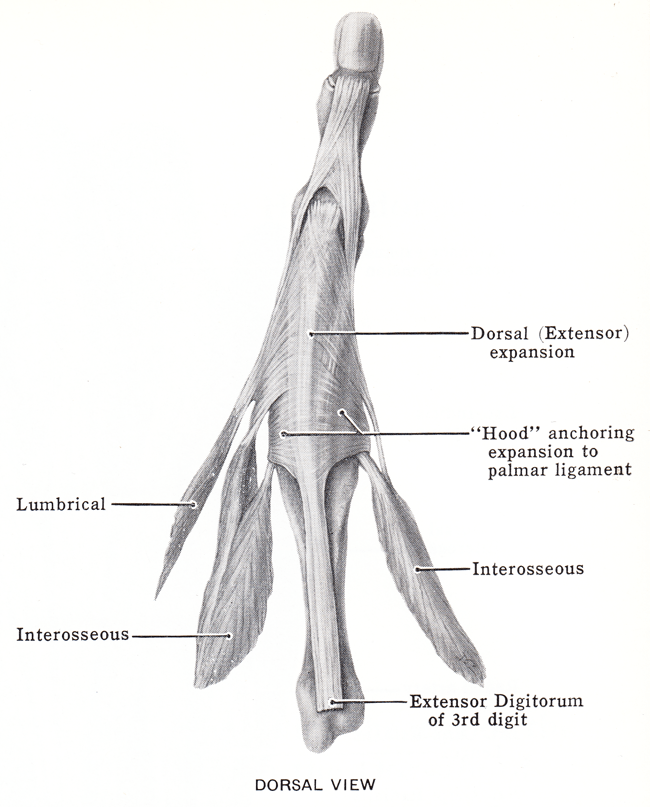
Here we see all the pieces that make up the extensor mechanism, which combines hand extrinsic and intrinsic muscles.
Let’s start with extensor digitorum communis (EDC), which acts to extend the MCPJ. This guy runs centrally along the finger, and splits off into sagittal bands that surround and stabilize the MPJ. In the picture, these would be a part of the “hood.”
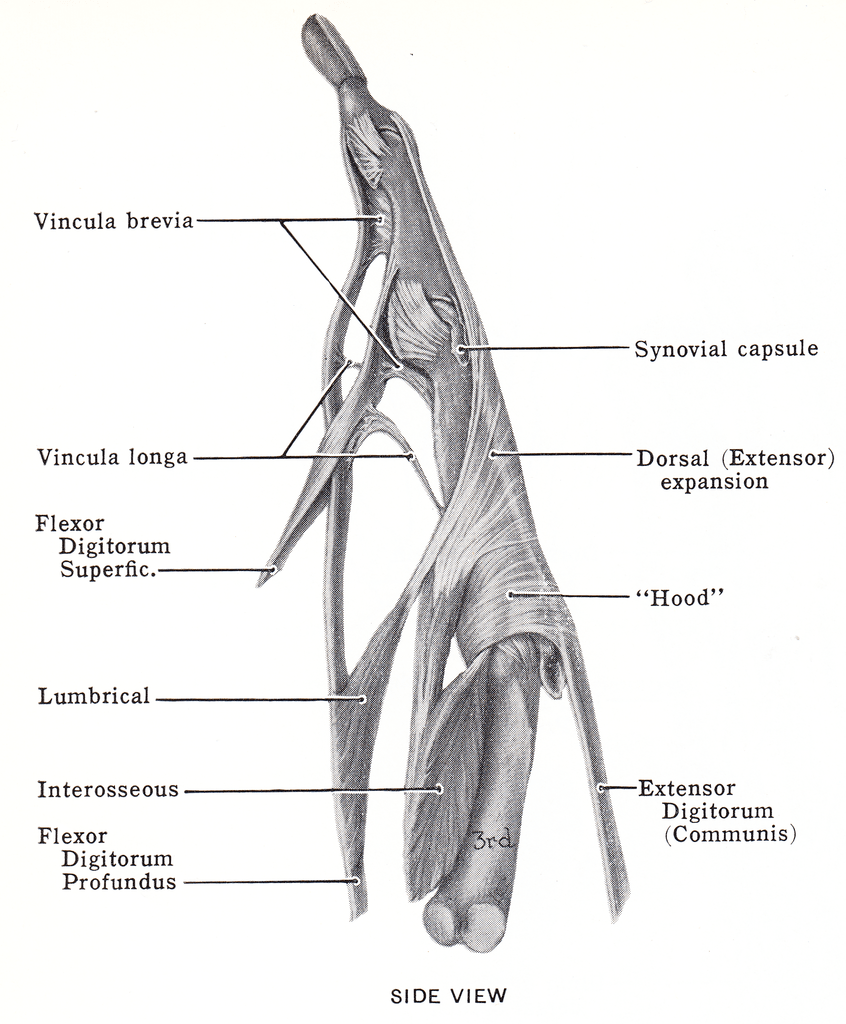
The EDC attaches to the middle phalanx, assisting with PIPJ extension. The fibers then split off into lateral bands, which are the criss crossed above past the middle phalanx. These bands are a merging with the hands intrinsic to perform DIPJ extension. The other muscles that would make up the lateral band insertion include the dorsal and palmar interossei, and the lumbricals—all helping to create DIPJ extension.
The Thumb
The big thumb intrinsic muscles are the called the thenar muscles, which help the thumb perform the important opposition movement. These include…
- Abductor pollicis brevis
- Flexor pollicis brevis
- Opponens pollicis
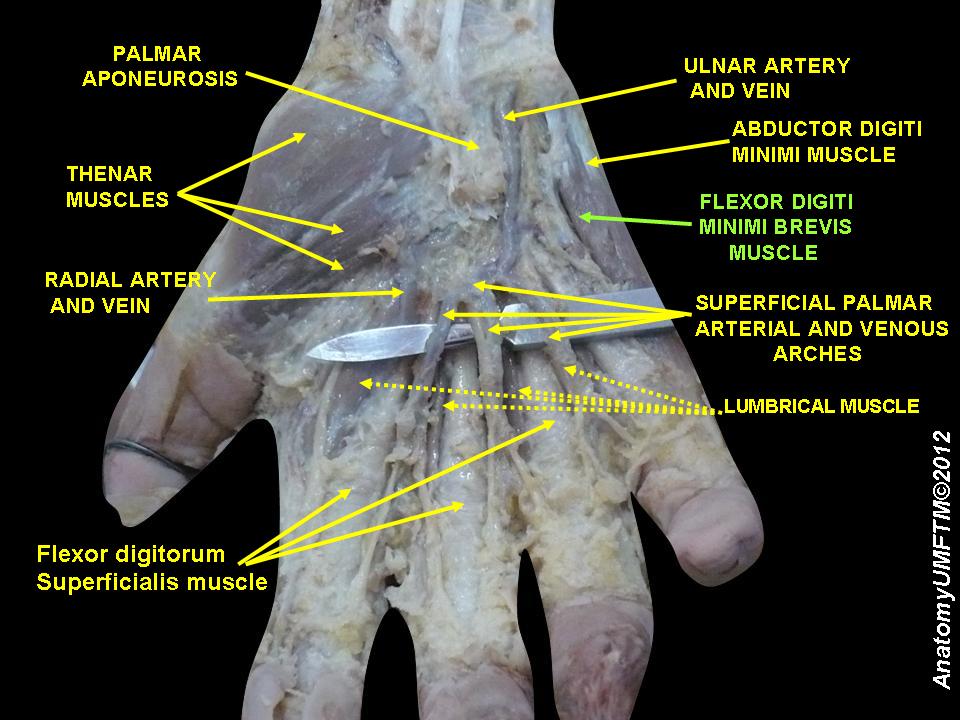
These muscles attach proximally at the volar carpal ligament. This attachment is important to consider with someone who has a carpal tunnel release, as this surgery disrupts the thenar muscle attachment, potentially compromising thumb function.
Nerve Supply to the Hand
The big three nerves relevant to the hand are the median, ulnar, and radial nerve.
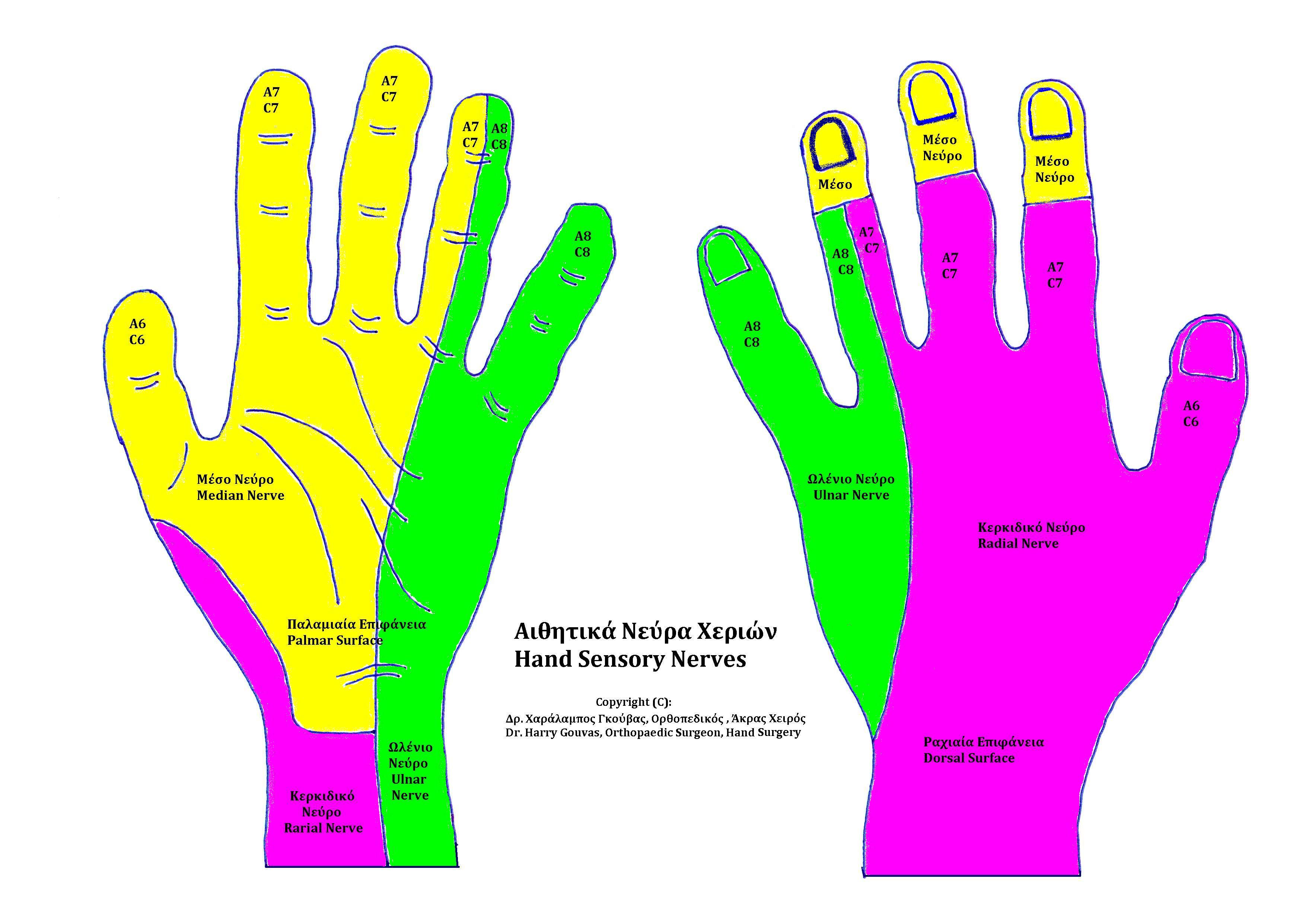
The median nerve is the big dog when it comes to thenar muscles and first two lumbricals. Injury to this nerve will impact thumb opposition and sensation.
The ulnar nerve innervates many of the muscles of the hand, including lumbricals 3 and 4, all the interossei, and the hypothenar muscles. Thus, an injury to this nerve can have severe repercussions to hand function. Limitations could include inability to perform a lateral pinch (requires adductor pollicis activity), can’t abduct finger V (need abductor digiti minimi), and will have difficulty utilizing extensor mechanism.
The radial nerve is less of a big dog, predominantly responsible for sensation. There will be alterations in wrist and finger extension, but since hand intrinsics are innervated by the median and ulnar nerve, some finger extension is preserved.
Common Hand Pathologies
Ever seen a swan neck or boutonniere deformity before?
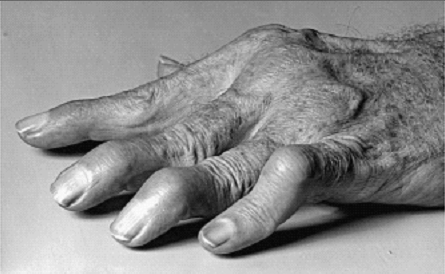
With a swan neck deformity, the proximal interphalangeal joint (PIPJ) upwardly displaces secondary to a disrupted transverse retinacular ligament. These ligaments prevent dorsal displacement of the lateral bands.
With the boutonniere deformity, a PIP extensor tendon defect causes the proximal phalanx to migrate upwardly as the DIPJ extends.
The de facto treatment for the boutonniere is splinting the PIPJ in extension and the DIPJ in flexion.
Evaluation of the Hand
Most of this section was your typical evaluation fare: history, range of motion, posture, palpation, etc. But there were a few key pearls I gleaned.
Measuring Thumb Opposition
Measuring opposition according to this grading system is something I am employing much more. We measure opposition via a 10-point grading criteria:
- Stage 0 – Thumb tip to lateral aspect of proximal phalanx of index finger
- Stage 1 – Thumb tip to lateral aspect of middle phalanx of index
- Stage 2 – Thump tip to lateral aspect of distal phalanx of index
- Stage 3 – Thumb tip to index tip (considered early true opposition)
- Stage 4 – Thumb tip to middle tip
- Stage 5 – Thumb tip to ring tip
- Stage 6 – Thumb tip to small tip
- Stage 7 – Thumb tip crosses small finger DIPJ
- Stage 8 – Thumb tip crosses small finger PIPJ
- Stage 9 – Thumb tip crosser small finger proximal finger crease
- Stage 10 – Thumb tip crosses distal palmar crease.
With stages 6-10, you want to make sure that the thumb slides down the small finger to ensure accurate opposition, as patients can compensate with thumb adduction, providing a false measure.
Sensation Return After an Injury
There are many ways to assess post-injury nerve function. One test used is tinel’s, in which you tap along the nerve to determine nerve regeneration. If you tap a portion of the nerve, it will produce an electric shock sensation to the point where the nerve has regenerated. This test can also signify potential nerve entrapment.
Based on how the nerve heals, constant and moving touch are some of the first sensations to return. Until these sensations are felt, true sensory re-education cannot be performed.
Wound Classificiations
A weak spot of mine has always been wound care. Patricia helped stratify decision making for wounds in this class by classifying wound healing types. There are three.
First Intention
This type of wound is a sutured wound, in which range of motion across joints that may compromise the wound ought to be limited for 2 weeks after initial suturing.
Second Intention
This type of wound is an open wound, in which the treatment varies. The intent is to maintain a wound that is not too dry or wet.
Third Intention
This wound is intentionally left open at first to clean and debride, then is sutured and grafted once healed. Treat as a second intention wound until suturing/grafting occurs, then first intention once the wound is closed.
Scar Healing Times
Scars have a specific healing times as well in the hands, which drive decision making in terms of progressing range of motion.
Coloring can be informative of how well the scar is healing. Typically, the redder the scar, the more immature the tissue is. Whereas white scars are a bit more mature.
Compared to normal skin, scar strength improves according to the following timeline:
- 2 weeks:3-5%
- 3 weeks = 15% (tolerates AROM)
- 4 weeks = 30-50% (safe for most activities)
- 2 months (70%)
- 3-6 months (80%).
Splinting the Hand
The splinting section was one of my favorite aspects of the course and really where Patricia shined.
The overarching goal of splinting is to give the hand what it cannot achieve.
Splints can be classified into three different types, either prefabricated or custom:
- Static – These splints lack moving parts, used for rest, protection, positioning, or function in some cases (e.g. nerve injury).
- Serial static/static progressive – These splints are used to increase mobility in joints and soft tissues via low load long duration stretching. The former requires therapist-remolding, whereas the latter is changed by modifying components (screw/Velcro)
- Dynamic – Splints that contain moving parts to compensate for motor loss, correct for contracture, protect tendons (by pulling in direction they cannot actively contract), or exercise muscles.
There were several different types of splints she suggested, but the real treat was watching her make splints. She had developed some pretty neat tricks to save on cost and maximize function. I don’t necessarily have any specifics, as the splints she makes were quite customized to the individual’s needs.
The Ideal Position to Splint the Hand
To illustrate important components of hand anatomy, it helps to look at how the hand is often splinted after an injury.
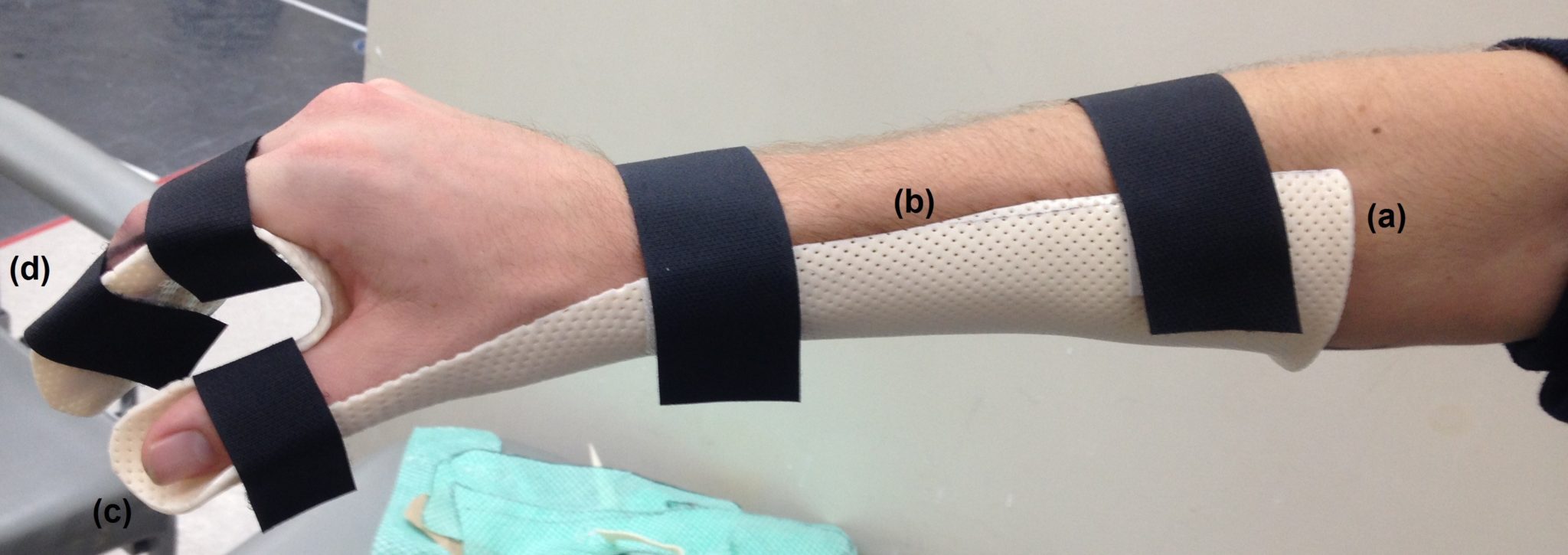
The common position to splint the fingers in is with the MCPJ in flexion, and the PIPJ and DIPJ in extension.
This position maintains tautness of all the collateral ligaments of each joint: the MPJ collaterals are taut in flexion, and the PIPJ and DIPJ in extension. This position also protects the volar plate, which is a ligamentous structure that limits PIPJ hyperextension. These structures must be preserved at all costs to avoid contracture in these areas.
Sum Up
There is a broad overview of Patricia’s Intro to Hand Therapy course. Though not perfect, it sparked many treatment ideas for me and helped me better appreciate the complexity of the hand.
To summarize:
- Understanding hand anatomy is important in developing treatment paradigms
- Flexor tendons must be differentially glided to ensure health post-surgery
- Splinting acts to give the hand functions it cannot achieve on its own
What tricks do you have up your sleeve for assessing and treating hand complaints? Comment below and let us know!